***LISTEN TO THE PODCAST HERE***
Guest
Michelle Brown, PhD, MS, MLS(ASCP)SBB
Assistant Professor and Director, Healthcare Simulation Graduate Program
University of Alabama at Birmingham
Transfusion Statistics
According to the American Red Cross:
- Someone in the US needs blood every 2 seconds
- 36,000 units PRBC, 10,000 units of FFP, and 7,000 units of platelets are transfused every day in the US
- Over 21 million blood components are transfused each year in the US, but only 13.6 million are collected
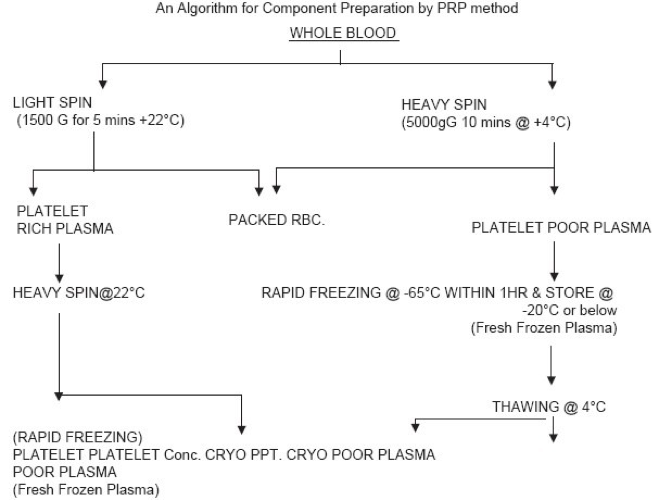
Process of Separation
When a person donates blood, 1 pint of whole blood is removed and then needs to be separated into its components for longer shelf life and targeted treatments. There are 2 processes on how this occurs:
- Platelet-Rich Process (PRP)
- Once the separation occurs, then the components can be treated with additives to help with viability and longevity. In the case of FFP and cryo, it is frozen to maintain potency of coagulation factors.
Packed Red Blood Cells
- Facts
- One unit of PRBC = 300cc
- Hematocrit = 55-80%
- One of PRBC should raise hemoglobin by 1g/dL and hematocrit by 3%
- Storage Considerations
- Can be stored for up to 42 days
- Treated with citrate to prevent clotting
- Indications for Transfusion
- Recommendations from 2016 AABB Guidelines
- ***To pair with patient symptoms***
- Hemodynamically-stable, restrictive threshold = Hgb < 7g/dL
- Orthopaedic surgery, cardiac surgery, or patients with CV = Hgb < 8g/dL
- Recommendations from 2016 AABB Guidelines
- Complications
- Hypocalcemia
- Transfusion reactions
- Alloimmunization
Fresh Frozen Plasma
- Facts
- 1 unit of FFP = 250cc
- Contains all coagulation factors
- Has an INR ~ 1.6
- Storage Considerations
- Frozen to -18-30oC within 8 hours of collection
- Takes 10-30 minutes to thaw
- Properly stored for up to 1 year
- Must be used within 5 days after thawing
- Frozen to -18-30oC within 8 hours of collection
- Indications for Transfusion
- Vitamin K factor deficiency
- Supratherapeutic vitamin K antagonist therapy
- Liver disease
- Massive transfusion protocol
- DIC
- TTP
- Vitamin K factor deficiency
- Not indicated for hypovolemia and low BP
- Complications
- Male only plasma à decreases in TRALI
Cyoprecipitate
- Facts
- Precipitant that forms after FFP is frozen and thawed at 4oC
- 1 unit of cryoprecipitate = 10-20cc
- Contains fibrinogen, factor VIII, XIII, and vWF
- Storage
- Re-frozen at -18oC
- Takes 10-30 minutes to thaw
- Stored for up to 1 year
- Only good for 4 hours once thawed and pooled, so order only when you need to transfuse
- Re-frozen at -18oC
- Indications for Transfusion
- Low fibrinogen due to:
- DIC
- Liver disease
- Uremia
- Inherited disorders of fibrinogen
- Low fibrinogen due to:
- Complications
- Same as other blood products
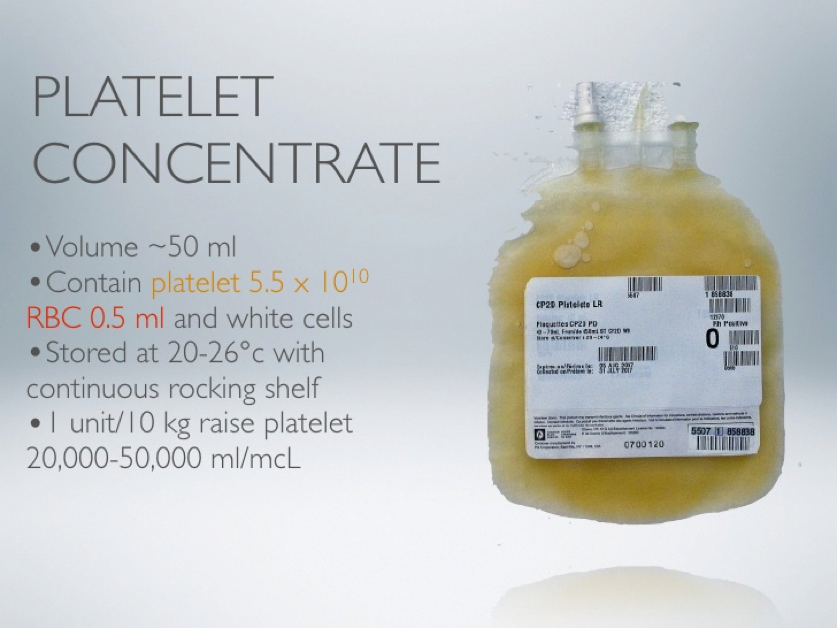
Platelets
- Facts
- 2 collection types
- Pooled
- Centrifuged down from whole blood
- Combined with other donors
- Apheresis (single donor)
- Platelets collected from donor and RBC and plasma returned
- Allows matching
- Volume ~300cc
- Six-pack of pooled or one unit of apheresed platelet should raise platelet count by 30-60,000/uL
- Pooled
- 2 collection types
- Storage
- Stored at room temperature because cold induces clustering of vWF receptor
- Only a 5-day shelf life
- Indications for Transfusion
- Actively bleeding patients with thrombocytopenia
- Prevention of spontaneous bleeding
- Varies depending on clinical condition
- < 10,000/uL
- No longer recommended to transfuse prophylactically when patient is on bypass – only is patient exhibits bleeding w/ thrombocytopenia or plt dysfunction
- Preparation for invasive procedures:
- Neurosurgery or ocular surgery – 100,000/uL
- Most major surgery – 50,000/uL
- Central line placement – 20,000/uL
- Lumbar puncture – 50,000/uL
- Epidural anesthesia – 80,000/uL
- Complications
- Increased infection risk
Component Modification Techniques
Leukoreduction
- Indicated for:
- Chronically transfused patients
- Solid organ or bone marrow transplant patients
- Previous febrile non-hemolytic reaction
Irradiated
- Irradiation inactivates lymphocytes
- Decreased risk of Graft-versus-host disease in immunocompromised patients
- Reduces shelf life to 28 days
Washed
- Rinsing serum proteins away prior to transfusions
- Indicated for severe or recurrent allergic reactions and IgA deficiency
- Indicated if a patient (especially neonate) is hyperkalemic
CMV-Negative
- Indicated for immunocompromised patients
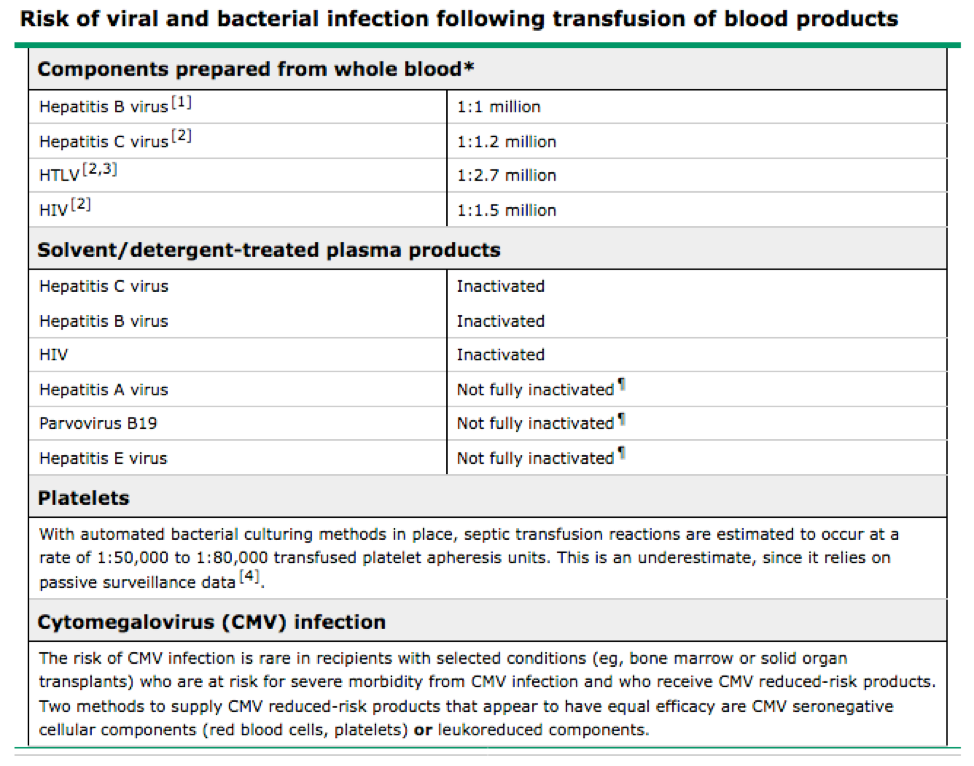
Transfusion Related Complications
References
- American Red Cross. Blood Facts and Statistics. http://www.redcrossblood.org/learn-about-blood/blood-facts-and-statistics. Accessed 03/23/2017.
- Brown MR, Jennings PR. Avoiding overtransfusion: an update on risks and latest indications. JAAPA. 2012;25(8):42-5. [pubmed]
- Basu D, Kulkarni R. Overview of blood components and their preparation. Indian J Anaesth. 2014;58(5):529-537. [pubmed]
- Carson JL, Guyatt G, Heddle NM. Clinical Practice Guidelines From the AABB: Red Blood Cell Transfusion Thresholds and Storage. JAMA. 2016;316(19):2025-2035. [pubmed]
- Life In The Fastlane. Fresh Frozen Plasma. https://lifeinthefastlane.com/ccc/fresh-frozen-plasma-ffp/. Accessed 03/23/2017.
- Roback JD, Caldwell S, Carson J. Evidence-based practice guidelines for plasma transfusion. Transfusion. 2010;50(6):1227-39. [pubmed]
- Kaufman RM, Djulbegovic B, Gernsheimer T. Platelet transfusion: a clinical practice guideline from the AABB. Annals of internal medicine. 2015;162(3):205-13. [pubmed]
- Sharma S, Sharma P, Tyler LN. Transfusion of blood and blood products: indications and complications. American family physician. 2011;83(6):719-24. [pubmed]
- Takpradit K. Rational use of Blood Components. https://www.slideshare.net/tarlabgab/rational-use-of-blood-component/16. Accessed 03/23/2017.