Question
A 38yo G2P0202 Caucasian woman, with a BMI of 32, presents to your office for evaluation of a “spot” on her breast that she is concerned about. She explains that her great aunt was diagnosed with breast cancer last year at the age of 62 and she is worried. She has not noticed it before, but upon further inquiry states she does not perform self-breast exams very often. She is not currently using any form of contraception (husband has had a vasectomy), but reports using oral contraception pills from age 17-28. She describes her cycle history as regular for her occurring every 28-30 days, lasting 4-5 days with moderate bleeding. She denies any history of abnormal Pap results or any other cancer.
Past Medical History – Hypertension, Anxiety
Medications – Lisinopril 10mg, Escitalopram 10mg
OBGYN History – Menarche at 13, 1st child at 29, 2nd child at 31, breastfed both children for 6 months
Social History – Never smoker, social alcohol
- What parts of her history are significant?
- What do you specifically want to assess for on your physical examination?
- What findings would be considered benign and what would be considered concerning?
Answer
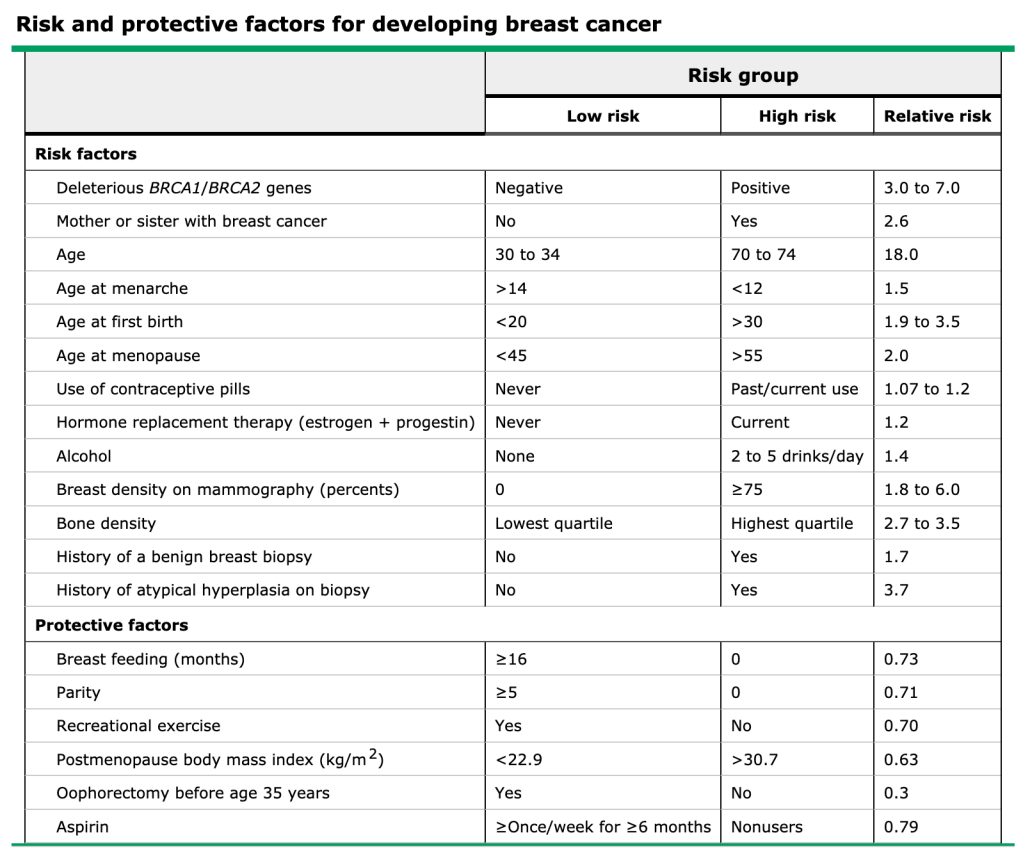
- The significant parts of her history are the use of estrogen-containing OCPs alcohol use, and age at time of first child as these have been associated with increased risk of breast cancer. Breastfeeding is actually protective against breast cancer. Her aunt (2nd degree relative) being diagnosed with breast cancer at 62, would only be significant if she was a 1st degree relative under 60 years of age.
- Physical examination should include:
- Inspection – asymmetry, skin changes, and nipple abnormalities
- Palpation – in a systematic approach with careful attention to the axillary lymph nodes and tail of the breast tissue
- Benign masses generally do not skin changes, are smooth, soft to firm, and mobile with well-defined margins. Malignant masses are generally hard, immobile, and fixed to the surrounding skin with poorly-defined margins.