#BOOM
Month: March 2016
Answer to Heme/Onc Questions
Question #1
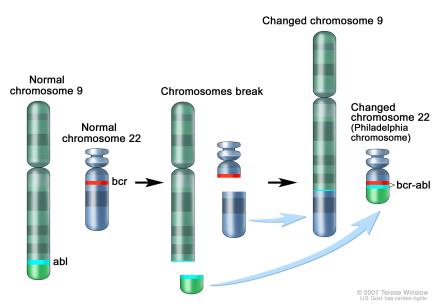
Which of the following genetic mutations is seen with chronic myelogenous leukemia?
Answer:
Translocation of chromosome 9 and 22. This new chromosome 22 is called “Philadelphia chromosome” after the city where the two hospitals that first identified the gene mutation in 1960 were both located.
Question #2
Which of the following cancer markers are classically associated with ovarian cancer?
Answer:
CA-125
#10 – Approach to Anemia in Adults
Definition
The textbook definition of anemia is a reduction of the absolute number or mass of circulating red blood cells. This then causes a global reduction in the oxygen carrying capacity of the patient’s circulatory system. Clinically, we use hemoglobin and hematocrit as the surrogate markers and define anemia as 2 SD below the mean for gender:
- Men
- Hemoglobin < 13.5 g/dL
- Hematocrit < 41%
- Women
- Hemoglobin < 12.0 g/dL
- Hematocrit < 36%
- Special Populations
- Athletes
- May have a baseline anemia due to:
- Dilution from increased plasma volume
- Hemolytic breakdown from exercise
- Exercise induced cytokines decreases RBC production
- A normal H/H in a competitive athlete may suggest performance enhancing drugs
- May have a baseline anemia due to:
- High altitudes
- May have elevated hemoglobin concentration as baseline
- Smokers
- Baseline higher hemoglobin due to carboxyhemoglobin
- Athletes
General Causes of Anemia
There are two general approaches you can use to help identify the cause of anemia in adults.
- The Kinetic Approach (the mechanisms responsible for the low hemoglobin)
- 3 independent mechanisms
- Decreased RBC production
- Lack of nutrients
- Bone marrow failure
- Decreased erythopoetic stimulation factors
- Erythropoietin, T3, androgens
- Inflammation
- Increased RBC destruction
- Hemolysis, hypersplenism
- Blood loss
- Decreased RBC production
- 3 independent mechanisms
- The Morphologic Approach (categories based on RBC size and reticulocyte response)
- Macrocytic (MCV > 100 fL)
- Vitamin B12, folate, EtOH, liver disease
- Any condition causing reticulocytosis
- Microcytic (MCV < 80 fL)
- 3 most common in clinical practice
- Iron deficiency
- ↓ serum iron, ↓ serum ferritin, ↑ TIBC
- Alpha or beta thalassemia minor
- Normal iron studies
- Anemia of chronic disease
- ↓ serum iron, normal serum ferritin, ↓ TIBC
- Iron deficiency
- 3 most common in clinical practice
- Macrocytic (MCV > 100 fL)
History Questions
- Is the patient symptomatic?
- Fatigue, dyspnea, bleeding, bruising, dizziness, syncope
- Any history of weight loss, night sweats, fever, anorexia?
- Infection or malignancy
- Past medical history for chronic illness
- PUD, renal disease, autoimmune conditions, liver disease, past malignancies
- Family history for hemoglobinopathies
- Social history for alcohol use
- Occupational exposures
Physical Exam Findings
- Pallor
- Palms, nail beds, face, conjunctiva
- Jaundice
- Hepatosplenomegaly
- Lymphadenopathy
- Petechiae, purpura, bruising
- Bone tenderness
Laboratory Testing
Anemia is usually first diagnosed by CBC. Once you have a documented low H/H, then you need order follow-up studies to help differentiate the cause of the anemia. These include:
- RBC indices
- MCV, MCH, MCHC, RDW
- Reticulocyte count and index
- Peripheral smear
- Helmet cells or schistocytes à microangiopathic hemolysis
- Microspherocytes à autoimmune hemolysis
- Tear drop RBC à myelofibrosis
- Bite cells à oxidative hemolysis
- Parasites à malaria, babeosis
- Hypersegmented neutrophils à Vitamin B12 or folate deficiency
- Nucleated RBC
- Siderocytes
- Target cells à thalassemias
- WBC and platelet count from CBC
- If hemolysis is suspected:
- ↑ Serum LDH, ↓ serum haptoglobin, and ↑ serum indirect bilirubin
- Direct Coombs test (antibodies against RBC)
- Bone marrow evaluation

Schrier SL, et al. Approach to adults with anemia. In: Up To Date. Waltham, MA (Accessed 03/23/2016)
The Cottage Physician Management
Something new I thought I would bring to the PAINE Podcast. As you all know, I am quite a fan of medicine and antiquity. Shortly after I married my wife, her grandfather past away from a progressive esophageal cancer. One of the things I was able to keep when helping clean out his house, was a copy of The Cottage Physician printed in 1893. It was basically a handbook on how to treat common ailments of the time. I will try to add excerpts from this book when appropriate so you can have a sense of how medicine was practiced in the late 19th century.
References
- Patel KV. Variability and heritability of hemoglobin concentration: An opportunity to improve understanding of anemia in older adults. Haematologica. 2008;93(9):1281-1283.
- Beutler E, Waalen J. The definition of anemia: what is the lower limit of normal of the blood hemoglobin concentration?. Blood. 2006;107(5):1747-50.
- Shaskey DJ, Green GA. Sports haematology. Sports Med. 2000;29(1):27-38.
- Ruíz-argüelles GJ. Altitude above sea level as a variable for definition of anemia. Blood. 2006;108(6):2131.
- Nordenberg D, Yip R, Binkin NJ. The effect of cigarette smoking on hemoglobin levels and anemia screening. JAMA. 1990;264(12):1556-9.
- Hillman RS, Ault KA, Leporrier M, Rinder HM. Clinical Approach to Anemia. In: Hematology in Clinical Practice. 5th McGraw-Hill. New York. 2010.
- Tefferi A. Anemia in adults: a contemporary approach to diagnosis. Mayo Clin Proc. 2003;78(10):1274-80.
- Nardone DA, Roth KM, Mazur DJ, Mcafee JH. Usefulness of physical examination in detecting the presence or absence of anemia. Arch Intern Med. 1990;150(1):201-4.
- Hung OL, Kwon NS, Cole AE, et al. Evaluation of the physician’s ability to recognize the presence or absence of anemia, fever, and jaundice. Acad Emerg Med. 2000;7(2):146-56.
A Few Quick Ones
Answer to Hematology/Oncology Case #1
Answer:
Check a methylmalonic acid level
This patient has had a history of gastric cancer with a partial gastrectomy and now presents with a fatigue and gait disturbances. CBC reveals a macrocytic aneamia and peripheral smear shows multinucleated neutrophils. The gait disturbances are most likely due to the progressive peripheral neuropathy. This is most consistent with vitamin B12 deficiency. Intrinsic factor, which is secreted by the parietal cells of the stomach, is required for vitamin B12 absorption in the terminal ileum.
Work-Up for Vitamin B12 Deficiency
Serum B12 Level
- < 300 pg/dL is diagnostic
Metobolites
- Methylmalonic acid
- < 70 nanomol/L is diagnostic
- Homocysteine
- < 5 micromol/L is diagnostic
Possible additional testing in the setting of macrocytic anemia:
- If pernicious anemia is suspected:
- Anti-intrinsic factor antibodies
- If folate deficiency is suspected:
- Serum folate level
- < 2 ng/mL is diagnostic
- RBC folate level (reserved for indeterminate serum levels)
- < 280 ng/mL is diagnostic
- Serum folate level
Treatment for B12 Deficiency
- Intramuscular
- 1mg daily x 7 days, then 1mg weekly for 4 weeks, then 1mg monthly
- Oral
- 1000-2000mg daily
References
- Antony AC. Megaloblastic anemias. In: Hematology: Basic principles and practice, 4th ed, Hoffman R, Benz EJ, Shattil SJ, et al. (Eds), Churchill Livingstone, New York 2005. p.519.
- Butler CC, Vidal-alaball J, Cannings-john R, et al. Oral vitamin B12 versus intramuscular vitamin B12 for vitamin B12 deficiency: a systematic review of randomized controlled trials. Fam Pract. 2006;23(3):279-85.
Hematology/Oncology Case #1
62-year-old male presents to primary provider’s office with a six-month history of fatigue and gait disturbance. He denies recent falls, weakness, pain, paralysis, or dizziness.
Medications
Lisinopril 10mg daily
Metformin 1000mg BID
Men’s multivitamin
Fish oil
Past Medical History
Diabetes Mellitus II
Hypertension
Gastric cancer
Past Surgical History
Cholecystectomy – 1997
Partial gastrectomy – 2004
Vitals
BP-128/79, HR-81, RR-14, O2-100%, Temp-98.9o
Physical Exam
General – WN/WD, NAD
Skin – scattered senile purpura, no petechiae
CV – RRR without M/G/R
Pulmonary – CTA bilaterally without adventitial breath sounds
Neurologic – A&Ox3, 5/5 strength throughout bilaterally, DTR 2+ and equal, FROM, vibratory sensation decreased in bilateral lower extremities
Laboratory Studies
#9 – The CBC Demystified
***Listen to the podcast here***
White Blood Cell Count
- Normal range (4.0-11.0 x 103 cells/mm3)
- 2 Parts
- Actual count of the number of leukocytes in one cubic millimeter of blood
- Differential count (% of each of the 5 types of leukocytes)
- < 4.0 x 103 cells/mm3 = leukopenia
- Bone marrow failure, blood malignancies, infections
- > 11.0 x 103 cells/mm3 = leukocytosis
- Infections, inflammation, blood malignancies
- Differential
- Granulocytes
- Neutrophils (45-73%)
- Bands (3-5%)
- “Left shift”
- Absolute Neutrophil Count (ANC)
- (%PMN + %Bands) x WBC / 100
- < 1500 = neutropenia
- Eosinophils (0-4%)
- Basophils (0-1%)
- Neutrophils (45-73%)
- Non-granulocytes
- Lymphocytes (20-40%)
- 3 Main Types
- T-Cells = cell mediated immunity
- B-Cells = humoral immunity (immunoglobulins)
- Natural Killer Cells (NKC)
- 3 Main Types
- Monocytes (2-8%)
- Lymphocytes (20-40%)
- Granulocytes
Red Blood Cell Count
- Actual count of RBC in one cubic millimeter of blood
- Normal range
- Male (4.5-5.9 x 1012 cells/L)
- Female (4.1-5.1 x 1012 cells/L)
- Reasons for gender differences in RBC markers
- Blood loss from menstruation
- Testosterone is hematapoetic
- 2 main markers
- Hemoglobin
- Amount of Hgb contained in a given volume of blood
- Normal Range
- Male (14-17.5 g/dL)
- Female (12.3-15.3 g/dL)
- Hematocrit
- % of total blood volume made up by RBC
- Normal range
- Male (42-50%)
- Female (36-45%)
- As a general rule of thumb, most agreed upon transfusion trigger is Hgb < 7.0 g/dL and/or Hct < 20%
- Hemoglobin
- Normal range
Red Blood Indices
- Essentially assess the size and hemoglobin content of the RBC and is useful in the evaluation of anemias, polycythemias, and nutritional deficiencies
- Mean Corpuscular Volume (MCV)
- Average size of the volume of RBC (Hct/RBC count)
- Normal range (80-100 fL/cell)
- < 80 = Microcytic
- > 100 = Macrocytic
- Mean Corpuscular Hemoglobin (MCH)
- Average amount of hemoglobin within a RBC
- Closely resembles MCV and of little clinical use
- Mean Corpuscular Hemoglobin Concentration (MCHC)
- Calculation of Hgb/Hct
- Normal range (32-36 g/dL)
- < 32 = hypochromic
- > 36 = hyperchromic
- Red Blood Cell Distribution Width (RDW)
- Indication of RBC size variability (degree of anisocytosis)
- Normal range (11-14%)
- Reticulocyte Count
- Measure of immature RBC in circulation
- Evaluates bone marrow function and erythropoetic activity
- Normal range (0.5-2.5%)
- Reticulocyte Index
- Measures whether this response is appropriate
- Reticulocyte Count % x (Patient’s Hct/Normal Hct)
- < 1.0 = poor response
- Measure of immature RBC in circulation
Platelet Count
- Actual count of thrombocytes in one cubic millimeter of blood
- Normal range (150,000-450,000/µL)
- Mean Platelet Volume (MPV)
- Relationship between size and count
- Immature platelets are larger
- MPV is analogous to the MCV
Strategies for Quick Interpretation
- If abnormal WBC:
- Correlate with clinical picture
- An abnormal number may be a normal response to illness or a marker of illness severity
- Look at your differential
- If leukopenic, then calculate ANC
- Correlate with clinical picture
- If abnormal RBC:
- Is your patient symptomatic?
- Look at your indices
- Calculate reticulocyte count for response
- If abnormal platelet:
- Is the patient bleeding?
References
1) Pagana KD, Pagana TJ. Mosby’s Manual of Diagnostic and Laboratory Tests. 5th ed. St. Louis, MO. Elsevier. 2014.
2) Lee M. Basic Skills in Interpreting Laboratory Data. 5th ed. Bethesda, MD. American Society of Health-Systems Pharmacists. 2013
3) Laposata M. Laboratory Medicine: The Diagnosis of Disease in the Clinical Laboratory. 2nd ed. New York, NY. 2014.