Question
You are winding down your 8a-8p shift in the fast track section of your emergency department when a 19-month girl is brought in my her father after falling out of a shopping cart at Home Depot at around 7:15pm. Her father saw her fall and couldn’t catch her before she hit the ground. She immediately began crying and her father denies any loss of consciousness or vomiting. She cried for approximately 30 minutes and her father started to worry that she is now “sleepy”. Other than the sleepiness, her behavior has been normal per her father.
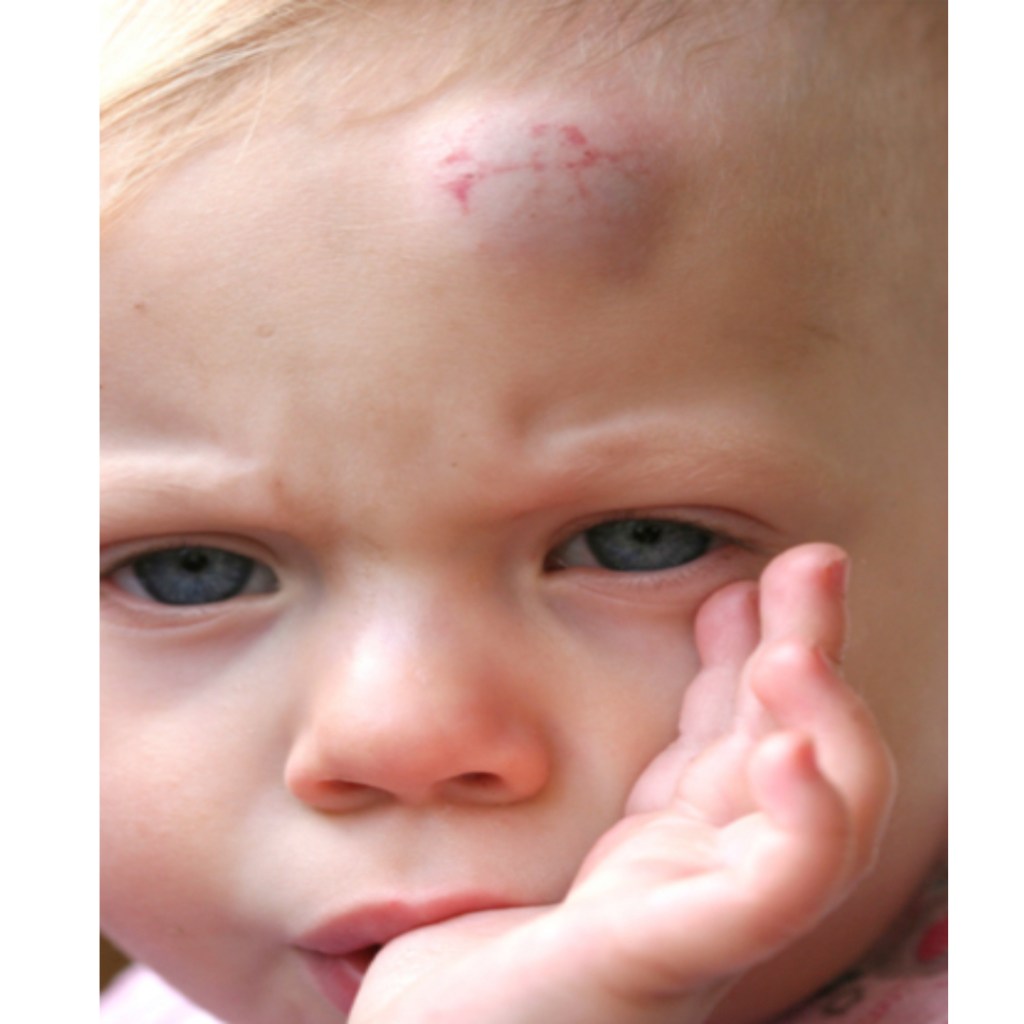
Physical examination does not reveal any periorbital or posterior auricular ecchymosis and there is no hemotympanum. There are no other abrasions or ecchymosis present and her eyes are open and she can track your movements. There is no palpable depressions or crepitus on the skull. She is moving all extremities, reaching for her toys, and saying “Daddy” towards her father.
- Does this child need further imaging?
- What studies are available to help make this decision?
Answer
This simple and most evidence-based answer is no…..not according to PECARN. The Pediatric Emergency Care Applied Research Network study of 2009 evaluated over 40,000 children of various ages to determine high yield clinical findings that best predicted clinically important traumatic brain injury on CT scan. The original negative predictive value in children under 2 with the following findings was 100%:
- Normal mental status
- No scalp hematoma (except frontal)
- No loss of consciousness, or < 5 seconds
- Non-severe mechanism of injury
- No palpable skull fractures
- Acting normal per parents

In our patient, you could make the argument to observe in the emergency department as she is “sleepy”, but it is close to bedtime and I would use shared decision making with the father to decide on discharge with good instructions vs observation for 4-6 hours.

References
- Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study. Lancet (London, England). 2009; 374(9696):1160-70. [pubmed]
- Schonfeld D, Bressan S, Da Dalt L, Henien MN, Winnett JA, Nigrovic LE. Pediatric Emergency Care Applied Research Network head injury clinical prediction rules are reliable in practice. Archives of disease in childhood. 2014; 99(5):427-31. [pubmed]
- Babl FE, Lyttle MD, Bressan S, et al. A prospective observational study to assess the diagnostic accuracy of clinical decision rules for children presenting to emergency departments after head injuries (protocol): the Australasian Paediatric Head Injury Rules Study (APHIRST). BMC pediatrics. 2014; 14:148. [pubmed]

