Genitourinary
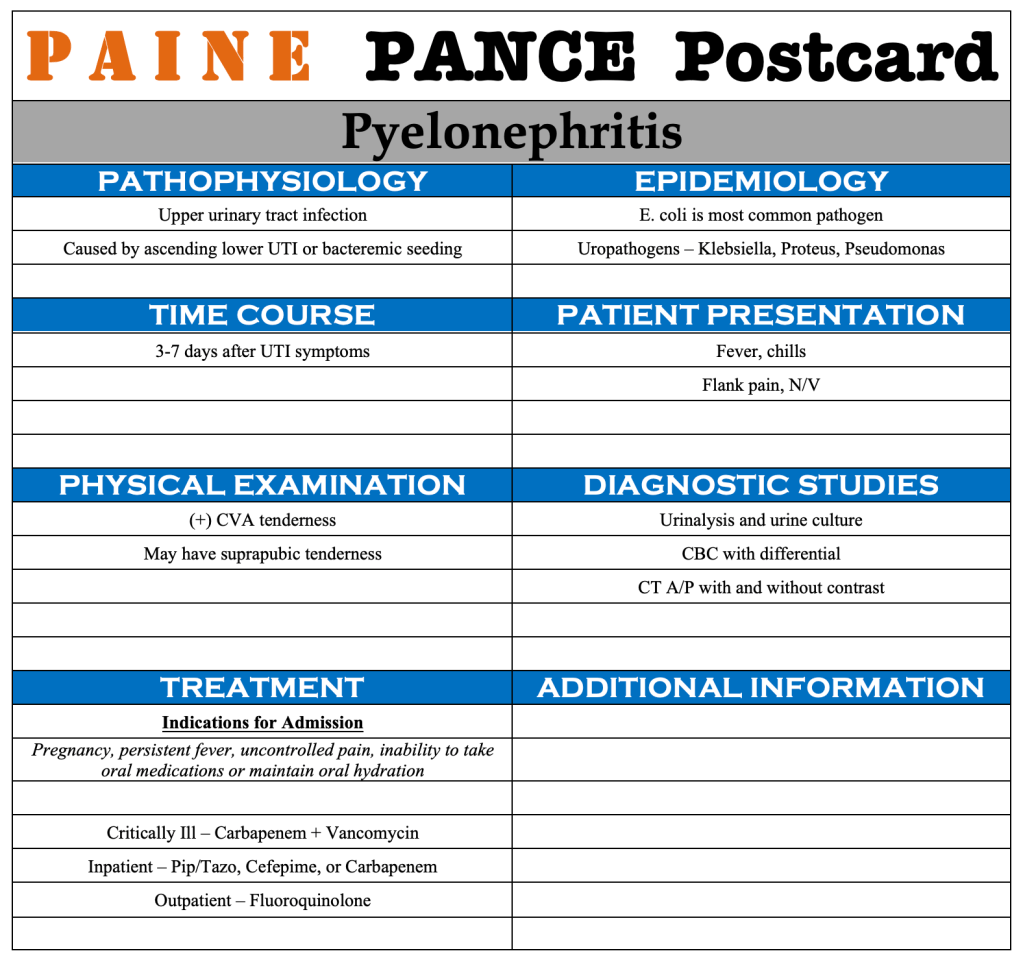
PAINE PANCE Postcard – Pyelonephritis

Urinary Incontinence
***LISTEN TO THE PODCAST HERE***

Nephrotic Syndrome
***LISTEN TO THE PODCAST HERE***
Ep-PAINE-nym
Bonney Test
Other Known Aliases – none
Definition – bedside test with urinary incontinence to determine if it is due to anatomical or structural issues
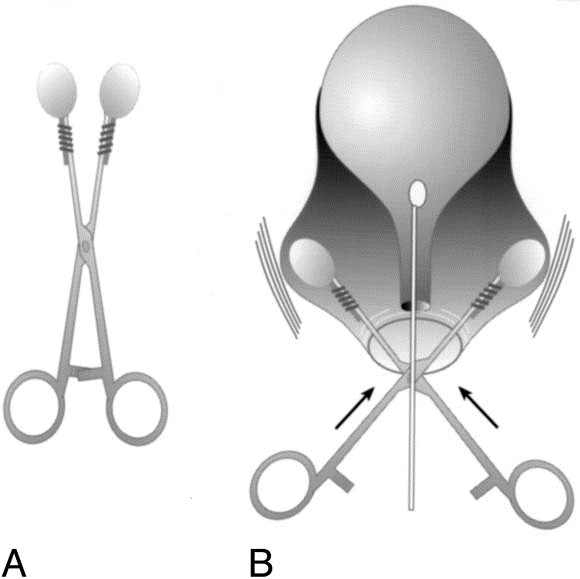
Clinical Significance – After a positive stress incontinence test, Bonney test is performed, where either a specialized instrument or examiner’s fingers are placed laterally to the urethral opening and pushed up to elevate the neck of the bladder. The patient then coughs to see if urine still escapes. If no urine leaks, then the incontinence is due the descent of the bladder neck into the vagina. If urine still escapes, it is due to weakness in the sphincter.
History – Named after William Francis Victor Bonney (1872-1953), a British gynecologist who received his medical doctorate from Chelsea Hospital for Women in 1896. He would go on to achieve Master of Surgery distinction in 1899 and was accepted as a fellow in the Royal College of Surgeons and Physicians in 1900. He would spend his entire career developing, pioneering, and mastering operative techniques in gynecologic surgery towards more conservative approaches to reduce mortality, morbidity, and disability associated with the more conventional approaches of the time. This was largely due to his wife, Annie, receiving a total hysterectomy early in their marriage for anemia associated with her heavy cycles. He also developed his own antiseptic solution called “Bonney’s Blue” used during vaginal surgeries which profoundly reduced infectious mortality. He would author more than 200 manuscripts during his career culminating his Textbook of Gynaecologic Surgery that is still in print today. He is regarded as one of, if not the, major influencer in modern gynecologic surgery.

References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Bonney, William Francis Victor (1872–1953). In: Baskett TF. Eponyms and Names in Obstetrics and Gynaecology . Cambridge University Press; 2019. [book]
- Powell, John L. MD, FACOG, FACS Powell’s Pearls, Obstetrical & Gynecological Survey: June 2005 – Volume 60 – Issue 6 – p 337-340 doi: 10.1097/01.ogx.0000162245.13467.5d
#64 – KDIGO Guidelines
***LISTEN TO THE PODCAST HERE***
What are KDIGO and KDOQI???
- The 2 Organizations
- Kidney Disease Outcomes Quality Initiative (KDOQI)
- US Based
- Developed in 1997 by National Kidney Foundation
- Kidney Disease: Improving Global Outcomes (KDIGO)
- Global organization developing and implementing evidence based clinical practice guidelines in kidney diseases
- Developed in 2003 by NKF
- Essentially individual entities, but both comment various aspects of kidney diseases
- Kidney Disease Outcomes Quality Initiative (KDOQI)
- 2012 Guidelines
- Published by KDIGO and commented by KDOQI
- 5 chapters
Chapter 1: Definition and Classification of CKD
- Definition
- Abnormalities in kidney structure or function, present for > 3 months, with implications on health





- Staging
- Based on causes, GFR category, and albuminuria category




- Predicting Prognosis of CKD

- Evaluation of GFR
- Recommend using serum creatinine and GFR estimating equation for initial assessment
- Recommend only using cystatin C in adult patients with decreased GFR but without markers of kidney damage if diagnosis of CKD is required

- Evaluation of Albuminuria
- Initial testing for proteinuria should be an early morning urine sample(in descending order of preference):
- Urine albumin-to-creatinine ratio (ACR)
- Urine protein-to-creatinine ratio (PCR)
- Reagent strip urinalysis for total protein with automated reading
- Reagent strip urinalysis for total protein with manual reading
- Microalbuminuria should no longer be used by laboratories
- If ACR > 30mg/g, then proceed to confirm with a random untimed urine sample
- Initial testing for proteinuria should be an early morning urine sample(in descending order of preference):
Chapter 2: Definition, Identification, and Predication of CKD Progression
- Assess albuminuria at least annually

- CKD progression is based on the one of the following:
- Decline in GFR category
- Drop in eGFR by ≥ 25% of baseline
- Sustained decline in eGFR by > 5mL/min/year
- Identify known risk factors associated with CKD progression
- Cause of CKD
- Age
- Gender
- Hypertension
- Hyperglycemia
- Dyslipidemia
- Smoking
- Obesity
- History of CVD
- Ongoing exposure to nephrotoxic agents
Chapter 3: Management of Progression and Complication of CKD
- Hypertension
- BP ≤ 140/90 if urine albumin excretion < 30mg/d
- BP ≤ 130/80 if urine albumin excretion > 30mg/d
- Recommend ACEI or ARB
- Protein Intake
- Recommend protein intake 0.8g/kg/d
- Glycemic Control
- Recommend HbA1C AROUND 7.0%
- ***newer ACE guidelines recommend < 6.5% with SGLT2i**

- Recommend < 2g/day
- Lifestyle
- Recommend 30 min/day five times per week, smoking cessation, and healthy weight (BMI 20-25)
- Lifestyle
- Complications Associated with CKD
- Anemia
- Diagnosed at < 13g/dL in men and < 12 g/dL in women
- Screening in patients with CKD:
- Stage G1-2 – when clinically indicated
- Stage 3a-3b – at least annually
- Stage 4-5 – at least twice per year
- Metabolic Bone Disease
- Obtained baseline calcium, phosphate, PTH, and ALP at least once in patients with GFR < 45 mL/min
- Not recommended to screen with bone mineral density testing
- Not recommended to supplement vitamin D of bisphophonates with deficiency or strong clinical rationale
- Acidosis
- Supplement oral bicarbonate in patients with serum bicarbonate < 22 mmol/L
- Anemia
Chapter 4: Other Complications of CKD
- CVD
- All CKD patients are at increased risk for CVD
- Recommend same testing and treating as non-CKD patients
- Use caution when interpreting NT-proBNP and troponins
- PVD
- Recommend regular podiatric assessment
- Medication Management
- Recommend using GFR for dosing adjustments
- Example – Metformin
- Stage G1-3a – continue
- Stage G3b – monitored
- Stage G4-5 – discontinued
- Example – Metformin
- Recommend using GFR for dosing adjustments

- Imaging studies and radiocontrast
- Avoid if possible, but do not hold if needed
- Following KDIGO Clinical Practice Guidelines for AKI
- Avoid high osmolar agents
- Use lowest contrast dose possible
- Stop nephrotoxic agents before and after
- Maintain adequate hydration
- Measure GFR 48-96 hours after
Chapter 5: Referral to Specialist and Models of Care



Cottage Physician (1893)

References
- KDIGO. Clinical Practice Guideline for the Evaluation and Management of CKD. 2012.
- Inker LA, Astor BC, Fox CH, et al. KDOQI US commentary on the 2012 KDIGO clinical practice guideline for the evaluation and management of CKD. Am J Kidney Dis. 2014; 63(5):713-35. [pubmed]
- Stevens PE, Levin A. Evaluation and management of chronic kidney disease: synopsis of the kidney disease: improving global outcomes 2012 clinical practice guideline. Ann Intern Med. 2013; 158(11):825-30. [pubmed]
- Andrassy KM. Comments on ‘KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease’. Kidney Int. 2013; 84(3):622-3. [pubmed]
PAINE #PANCE Pearl – Genitourinary
Question
This one is a quick one this week. When evaluating a patient with testicular pain (either acute or chronic), what are the specific physical examination techniques you can perform and what conditions do they help rule in/out?

Answer
- Position of the Testicle
- Side-lying (long axis transverse) position suggests testicular torsion
- also called the “Bell Clapper” deformity
- Side-lying (long axis transverse) position suggests testicular torsion
- Cremesteric Reflex
- Pinching the skin of the upper thigh causes elevation of testes
- If absent, suggests testicular torsion
- Pinching the skin of the upper thigh causes elevation of testes
- Blue Dot Sign
- Tender nodule with blue discoloration on the upper pole of the testes
- If present, suggests appendix testes torsion
- Tender nodule with blue discoloration on the upper pole of the testes
- Prehn Sign
- Manual elevation of testes relieves the pain
- If positive, suggests epididymitis
- Manual elevation of testes relieves the pain
- Transillumination
- In evaluating scrotal swelling, ability to transilluminate the scrotum suggests hydrocele.
- If unable to transilluminate, suggests varicocele or mass

Ep-PAINE-nym
Sertoli Cells
Other Known Aliases – none
Definition – sustentacular cell of the convoluted seminiferous tubule of the testes
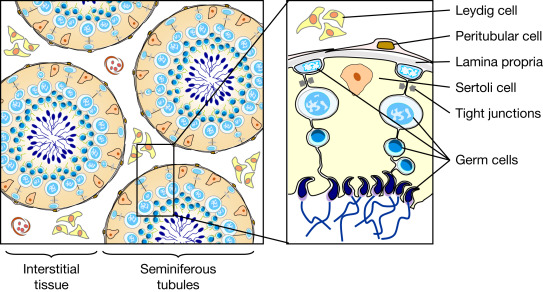
Clinical Significance – these cells are activated by FSH to produce and mature sperm during spermatogenesis
History – Named after Enrico Sertoli (1842-1910), who was an Italian physiologist and histologist and received his medical doctorate from the University of Pavia in 1865. His love and passion for histology was groomed while training under Eusebio Oehl, who was an early pioneer in microscopic anatomy and histopathology. He would go on to become professor of anatomy and physiology at the Royal School of veterinary medicine in Milan and it was here that he founded the laboratory of experimental physiology. In 1865, during his tenure in Milan, he published the paper describing his eponymous cell.

References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Sertoli E. Dell’esistenza di particolari cellule ramificate nei canalicoli seminiferi del testicolo umano. Morgagni, 1865; 7: 31-40
PAINE #PANCE Pearl – Genitourinary
Question
This one is a quick one this week. When evaluating a patient with testicular pain (either acute or chronic), what are the specific physical examination techniques you can perform and what conditions do they help rule in/out?

Ep-PAINE-nym
Fournier’s Gangrene
Other Known Aliases – none
Definition – necrotizing fasciitis of the external genitalia and/or perineum
Clinical Significance – this infection commonly affects older men and is associated with diabetes mellitus or a compromised immune system. Other risk factors include trauma or surgery to the perineal area, alcoholism, and childbirth. Pain, erythema, crepitus, and fever are common findings and treatment is aggressive surgical debridement and antibiotics to cover anaerobic and facultative pathogens.
History – Named after Jean Alfred Fournier (1832-1914), who was a French dermatologist and venereologist, and received his medical doctorate in 1860 while studying in Paris. He would begin his career as an understudy of Philippe Ricord at the Hôpital du Midi and would later become médecine des hôpitaux at the famed Hôtel-Dieu de Paris. It was in 1883 when he presented a case series of patients with gangrene of perineum and for which this eponym is attributed, although it was first described and published in 1764 by Baurienne. He is best known for his work with congenital syphilis (for which he has two additional eponyms) and advancing the study of venereal diseases and their connection to degenerative diseases.
References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Fournier, J.A. Gangrène foudroyante de la verge. La Semaine Médicale. 3 1883;(56): 345–347
- Toodayan N. Jean Alfred Fournier (1832-1914): His contributions to dermatology. http://www.odermatol.com/issue-in-html/2015-4-32/
- Waugh MA. Alfred Fournier, 1832-1914. His influence on venereology. Br J Vener Dis. 1974; 50(3):232-6. [PDF]