Question
A 3-week old baby girl is sent to your emergency department after being seen by their pediatrician for irritability, poor feeding, and a seizure just prior to arrival at the pediatrician’s office. Vital signs are BP-103/73, HR-137, RR-25, O2-100% on room air, and Temp-39.2oC (102.5oF). Physical examination reveals a lethargic infant with decreased motor tone and a full, bulging frontal fontanelle. What is the most important diagnostic study to obtain and what is the empiric treatment of choice while awaiting results?
Answer
- A full or bulging fontenelle is suggestive of meningeal edema and swelling are concerning for meningitis. Couple this with the lethargy and poor motor tone and this infant bought herself a lumbar puncture.
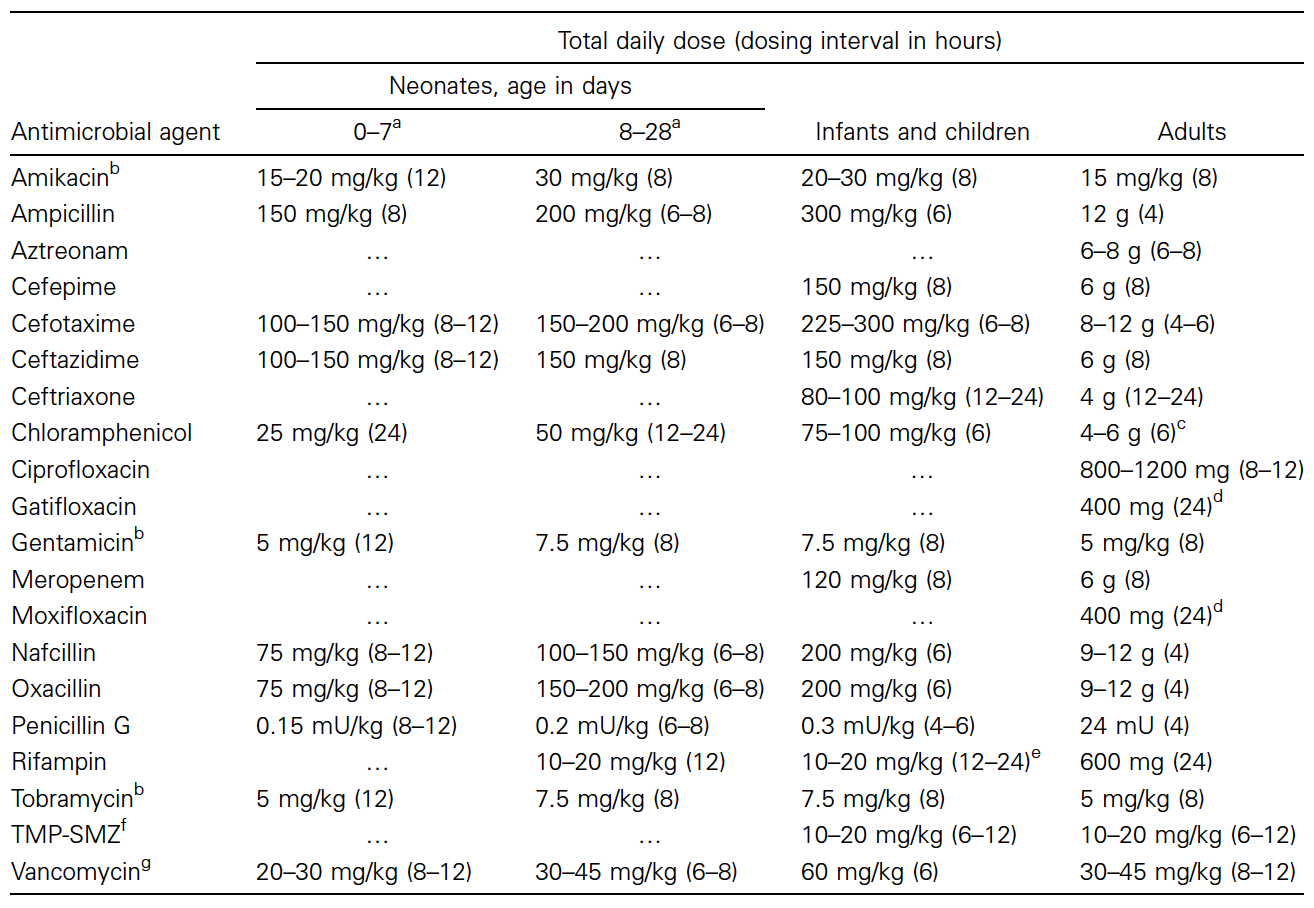
- Now….because of her age (<30 days old), you have to cover for a specific set of pathogens due to a developing immune system. Classically, neonatal sepsis bugs include group B streptococcus (GBS), Escherichia coli, and Listeria monocytogenes. Empiric antibiotic coverage (until gram stain results) is:
- Ampicilin (GBS)
- Gentamycin (gram negative coverage)
- Cefotaxime (wider gram negative coverage)