Neurologic
PAINE PANCE Postcard – Guillain-Barré Syndrome
PAINE PANCE Postcard – Febrile Seizures
Ep-PAINE-nym
Klumpke’s Palsy
Other Known Aliases – none
Definition – paralysis of the upper extremity from a lower trunk injury classically effecting C8-T1.
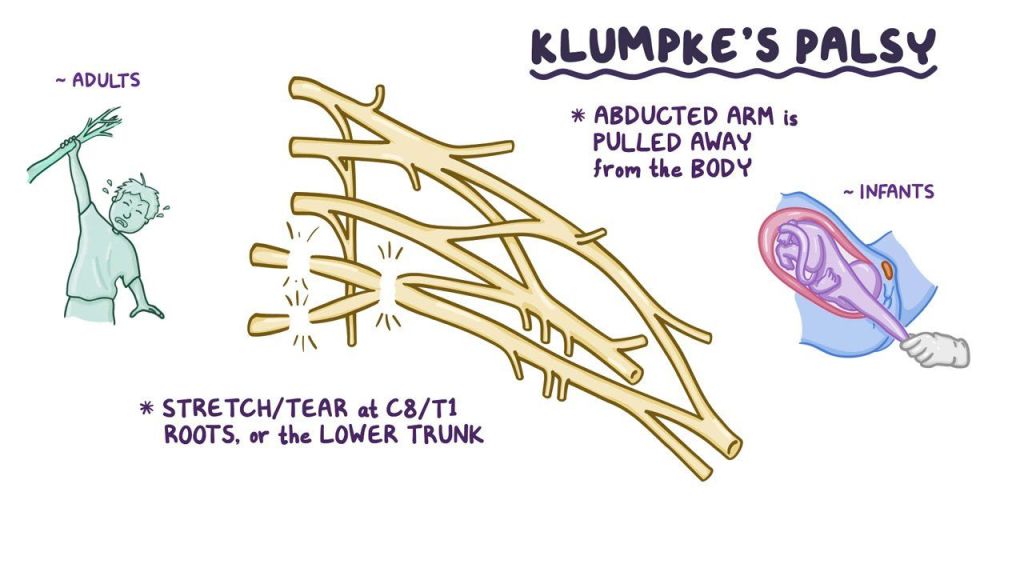
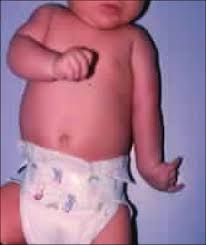
Clinical Significance – this brachial plexopathy can be infants as a result of birth trauma from pulling on an extending arm or in older children/adults from hanging from an outstretched arm. The classic manifestations are paralysis of the intrinsic hand muscles, fixed and flexed wrist and finger flexors, and sensory numbness of the C8/T1 dermatome leading to the textbook “claw hand” deformity.

History – Named after Augusta Déjerine-Klumpke (1859-1927), an American-born French physician who received her medical doctorate from the University of Paris in 1889 after becoming the first woman to be appointed interne des hôpitaux. She would immediately make a reputation for herself by being able to speak three languages and took an interest in neuroanatomy and physiology. She would meet fellow physician and future husband, Jules Dejerine, during her studies in medical school and the two would study and publish extensively together in the realm of neurology including the classic two-volume textbook on the anatomy of the nerve centers entitled “Anatomie des Centres Nerveux”. She would describe her eponymous condition in her 1885 case review of 18 patients taken from the available medical literature and would win her the Godard prize in 1886.
References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Yildirim FB, Sarikcioglu L. Augusta Dejerine-Klumpke (1859-1927) and her eponym. J Neurol Neurosurg Psychiatry. 2008; 79(1):102. [pubmed]
- Shoja MM, Tubbs RS. Augusta Déjerine-Klumpke: the first female neuroanatomist. Clin Anat. 2007; 20(6):585-7. [pubmed]
- Déjerine, JJ, Déjerine-Klumpke, A. Anatomie des Centres Nerveux. 1895. [link]
- Déjerine-Klumpke, A. Contribution à l’étude des paralysies radiculaires du plexus brachial. Paralysies radiculaires totales. Paralysies radiculaires inférieures. De la participation des filets sympathiques oculo-pupillaires dans ces paralysies. Revue de médecine 1885, 5: 591-616, 739-90.
#71 – Guillain-Barré Syndrome
***LISTEN TO THE PODCAST HERE***
DEFINITION
- Acute monophasic paralyzing illness usually provoked by a preceding event
- Most commonly this is an infection (2/3rds of patients)
- Other causes
- Immunizations
- Influenza, meningococcal (MCV4)
- Surgery
- Trauma
- Medications
- Immunizations
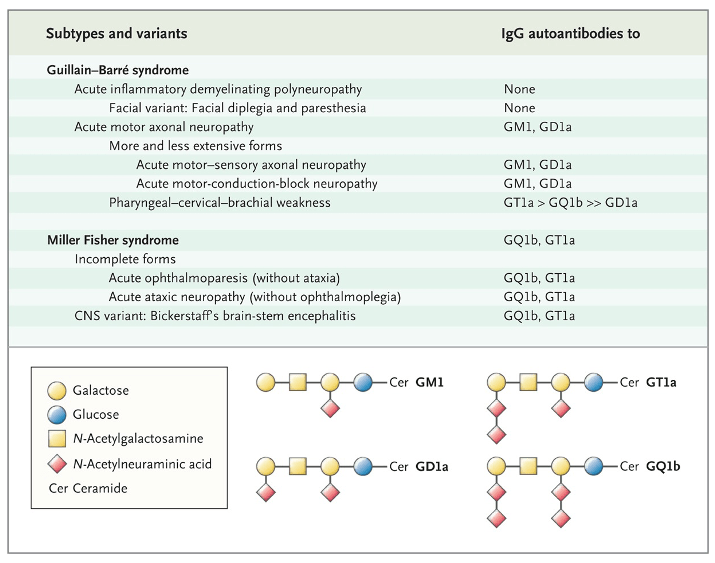
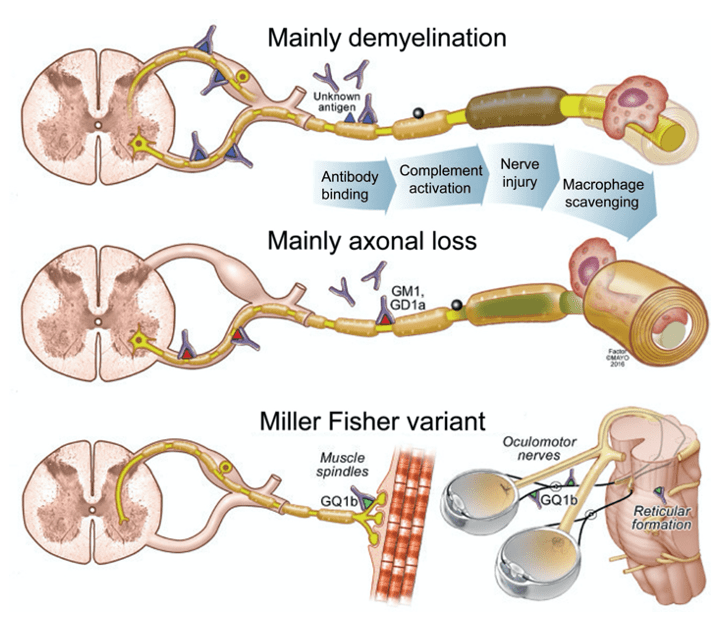
- Was considered to be a SINGLE condition, but now is recognized to be an umbrella term for a mix of many different variants
- Acute inflammatory demyelinating polyradiculoneuropathy (AIDP)
- Most common in the US (85-90%)
- Miller Fisher syndrome (MFS)
- Acute motor axonal neuropathy (AMAN)
- Acute sensorimotor axonal neuropathy (AMSAN)
- Acute inflammatory demyelinating polyradiculoneuropathy (AIDP)
EPIDEMIOLOGY
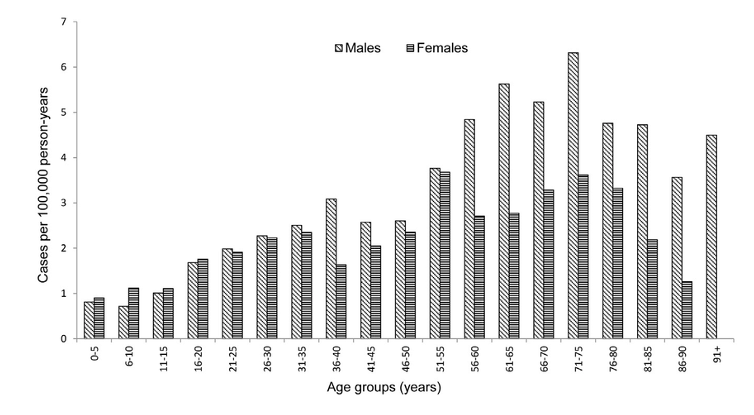
- 1-2 cases per 100,000 per year
- Incidence increases 20% with every 10-year increase in age after the first decade of life
- Slightly higher incidence in men than women
PATHOGENSIS
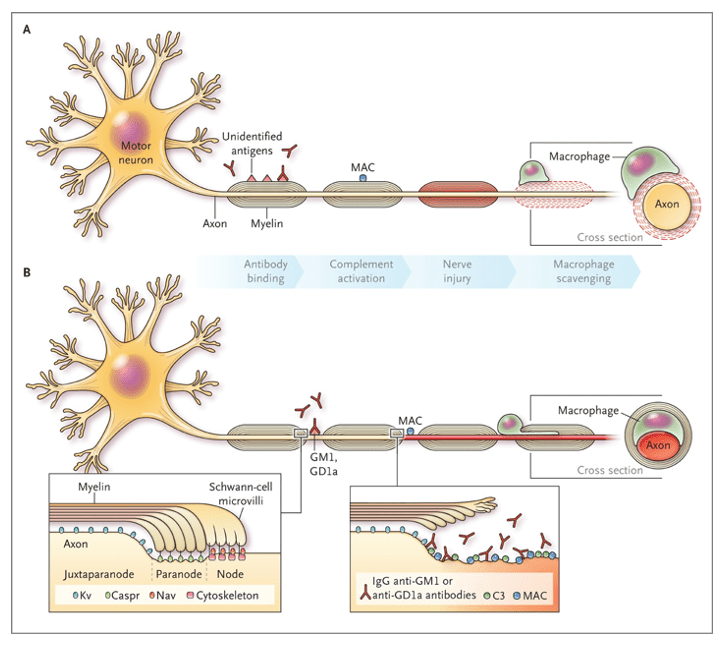
- Molecular Mimicry
- Antecedent event provokes an immune response, which produces antibodies that cross-reacts with nerve components due to the sharing of epitopes
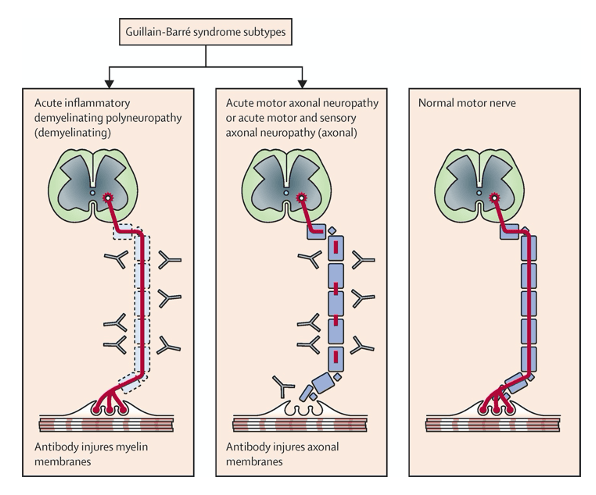
- If directed at Schwann cell surface membranes à AIDP
- Infiltration of lymphocytes in the epineural and endoneural veins causing myelin degeneration at the dorsal and ventral roots
- If directed at axonal membrane à AMAN and AMSAN
- Attack is directed at the nodes of Ranvier of the ventral roots of the peripheral nerves
- If directed at Schwann cell surface membranes à AIDP
- End result is blocking the neuro-electrical transmission of impulses
- Antecedent event provokes an immune response, which produces antibodies that cross-reacts with nerve components due to the sharing of epitopes
- Common infections
- C. jejuni (most common)
- HIV
- H. influenza
- M. pneumoniae
- CMV

CLINICAL FEATURES
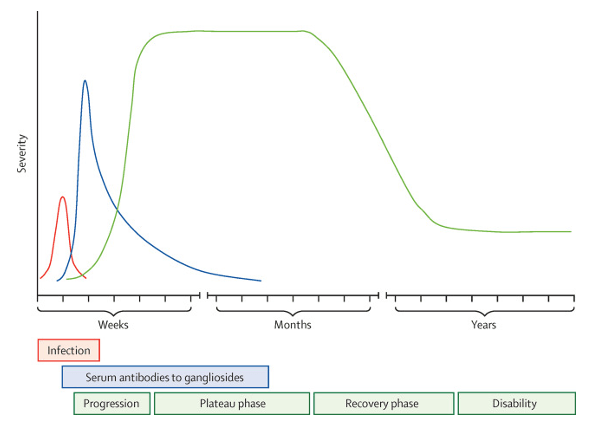
- Ascending (distal to proximal) symmetric muscle weakness with absent deep tendon reflexes progressing over days to weeks
- Weakness can vary from mild difficulty with walking to complete paralysis
- Symptom peak at around 4 weeks
- Respiratory dysfunction – 10-30%
- Facial nerve palsies or oropharyngeal weakness – 50%
- Oculomotor – 15%
- Paresthesias – 80%
- Dysautonomia – 70%
- Diarrhea, constipation, hyponatremia, bradycardia, urinary retention
- Variant Discrepancies
- AMAN – preservation of deep tendon reflexes
- AMSAN – more sensory disturbances
- Miller Fisher – ophthalmoplegia with ataxia and areflexia
DIAGNOSIS
- CSF Analysis
- Albuminocytologic dissociation
- Elevated protein with normal WBC
- Present within first week and peaks at 3 weeks
- Thought to be due to the increased permeability of the blood-nerve-barrier of the proximal roots
- Albuminocytologic dissociation
- Electrodiagnostic Studies (EMG and NCS)
- Demyelinating forms
- Decreased motor nerve conduction velocity
- Prolonged distal motor latency
- Complete conduction blocks
- Axonal forms
- Decreased distal motor and/or sensory amplitudes
- Serial studies can be helpful since the condition can progress over time
- Demyelinating forms
- Antibodies
- Specific autoantibodies can help differentiate variant subtypes
- MRI
- Thickening and enhancement of the intrathecal spinal nerve roots and cauda equina

DIAGNOSTIC CRITERIA
- Developed in 1978 and modified over the decades based on evolving research

TREATMENT
- Supportive care
- Respiratory support
- Up to 30% will require ventilatory support
- Impending respiratory arrest
- FVC < 20 mL/kg
- Maximum inspiratory pressure < 30 cmH2O
- Maximum expiratory pressure < 40 cmH2O
- Predictors of respiratory failure
- Time of onset to admission < 7 days
- Inability to cough, stand, lift elbows, or lift head
- Elevated LFTs
- Vital capacity < 60% predicted
- Online tool to help predict
- Autonomic Dysfunction
- Cardiovascular monitoring and support
- Hypertension and hypotension
- Bradycardia and tachydysrhythmias
- Bowel and Bladder care
- Urinary retention
- Ileus management
- Cardiovascular monitoring and support
- Respiratory support
- Disease-Modifying Treatment
- Started within 4 weeks of symptom onset
- Plasma exchange
- Remove circulating autoantibodies
- 4-6 treatments over 8-10 days
- Complications
- Hypotension, sepsis
- IVIG
- Interferes with production and function of cytokines, B-cells, and T-cells
- 0.4 grams/kg/day for 5 days
- Complications
- Meningitis, rash, renal failure

PROGNOSIS
- 60% will fully recover by 1 year
- 15% will have persistent severe motor problems
- 3-7% will succumb to the illness
- 20% of patients requiring mechanical ventilation
COTTAGE PHYSICIAN (1893)

REFERENCES
- Gibbons CH, Engstrom JW. Disorders of the Autonomic Nervous System. In: Jameson J, Fauci AS, Kasper DL, Hauser SL, Longo DL, Loscalzo J. eds. Harrison’s Principles of Internal Medicine, 20e. McGraw-Hill; Accessed May 09, 2021.
- Diseases of the Peripheral Nerves. In: Ropper AH, Samuels MA, Klein JP, Prasad S. eds. Adams and Victor’s Principles of Neurology, 11e. McGraw-Hill; Accessed May 09, 2021.
- Yuki N, Hartung HP. Guillain-Barré syndrome. N Engl J Med. 2012; 366(24):2294-304. [pubmed]
- Willison HJ, Jacobs BC, van Doorn PA. Guillain-Barré syndrome. Lancet. 2016; 388(10045):717-27. [pubmed]
- Sejvar JJ, Baughman AL, Wise M, Morgan OW. Population incidence of Guillain-Barré syndrome: a systematic review and meta-analysis. Neuroepidemiology. 2011; 36(2):123-33. [PDF]
- Alshekhlee A, Hussain Z, Sultan B, Katirji B. Guillain-Barré syndrome: incidence and mortality rates in US hospitals. Neurology. 2008; 70(18):1608-13. [pubmed]
- Fokke C, van den Berg B, Drenthen J, Walgaard C, van Doorn PA, Jacobs BC. Diagnosis of Guillain-Barré syndrome and validation of Brighton criteria. Brain. 2014; 137(Pt 1):33-43. [pubmed]
- Hadden RD, Cornblath DR, Hughes RA, et al. Electrophysiological classification of Guillain-Barré syndrome: clinical associations and outcome. Plasma Exchange/Sandoglobulin Guillain-Barré Syndrome Trial Group. Ann Neurol. 1998; 44(5):780-8. [pubmed]
- Lawn ND, Fletcher DD, Henderson RD, Wolter TD, Wijdicks EF. Anticipating mechanical ventilation in Guillain-Barré syndrome. Arch Neurol. 2001; 58(6):893-8. [pubmed]
- Raphaël JC, Chevret S, Hughes RA, Annane D. Plasma exchange for Guillain-Barré syndrome. Cochrane Database Syst Rev. 2012; [pubmed]
- Hughes RA, Swan AV, van Doorn PA. Intravenous immunoglobulin for Guillain-Barré syndrome. Cochrane Database Syst Rev. 2014; [PDF]
PAINE #PANCE Pearl – Neurology
Question
49yo man presents to his primary provider’s office with a 2-week history of bilateral leg weakness. He denies any pain associated with it and has never had any symptoms like this before. He denies any previous back problems and reports never remembers injuring his back. He thinks it first started in his feet when he noticed he was dragging is toes when walking, but now finds some difficulty lifting his legs when going up stairs. PMH is significant for hypertension (controlled on lisinopril) and osteoarthritis (controlled with exercise and celecoxib). He also reports having a pretty severe case of “food poisoning” a month ago when vacationing in the gulf, but is otherwise healthy.
Physical examination reveals 3/5 strength bilaterally with plantarflexion and dorsiflexion of the ankles and 4/5 strength bilaterally with hip and knee flexion. His ankle deep tendon reflex is absent and knee is diminished at 1+. Sensation and two-point discrimination of the feet are intact
- What would be the next step in the diagnostic evaluation of this patient?
- What is the most likely diagnosis and cause of this disease?

Answer
- Due to the acute nature of the symptoms and the absence of DTRs, Guillain-Barré Syndrome should be high on the differential. The next step should be performing an LP and performing a CSF analysis. Albuminocytologic dissociation (elevated protein with normal cell counts) is the hallmark of GBS.

Ep-PAINE-nym
Erb’s Palsy
Other Known Aliases – none
Definition – paralysis of the upper extremity from an upper trunk injury classically effecting C5-C6.

Clinical Significance – this brachial plexopathy is most commonly associated with birth trauma from a shoulder dystocia and depending on the severity of the injury, can resolve on its own or be permanent. The arm is classically internally rotated, with an extended and pronated forearm referred to as the “waiter’s tip” or “porter’s tip” sign.
History – Named after Wilhelm Heinrich Erb (1840-1921), a German neurologist who received his medical doctorate from the the University of Heidelberg in 1864. He would spend his early career assisting Nikolaus Friedreich and Ludwig von Buhl in Munich, before becoming chair of the pathology department at the University of Leipzig in 1880, and ultimately succeeding Friedreich in 1883. He is credited with popularizing the reflex hammer use in neurologic examinations and would be instrumental in identifying and describing myasthenia gravis, tabes dorsalis, and his eponymous point in the brachial plexus where this injury arises. Of note, he is also credited with the cardiac auscultation point where the S2 is best heard.
References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Sarikcioglu L, Arican RY. Wilhelm Heinrich Erb (1840-1921) and his contributions to neuroscience. J Neurol Neurosurg Psychiatry. 2007; 78(7):732. [PDF]
PAINE #PANCE Pearl – Neurology
Question
49yo man presents to his primary provider’s office with a 2-week history of bilateral leg weakness. He denies any pain associated with it and has never had any symptoms like this before. He denies any previous back problems and reports never remembers injuring his back. He thinks it first started in his feet when he noticed he was dragging is toes when walking, but now finds some difficulty lifting his legs when going up stairs. PMH is significant for hypertension (controlled on lisinopril) and osteoarthritis (controlled with exercise and celecoxib). He also reports having a pretty severe case of “food poisoning” a month ago when vacationing in the gulf, but is otherwise healthy.
Physical examination reveals 3/5 strength bilaterally with plantarflexion and dorsiflexion of the ankles and 4/5 strength bilaterally with hip and knee flexion. His ankle deep tendon reflex is absent and knee is diminished at 1+. Sensation and two-point discrimination of the feet are intact
- What would be the next step in the diagnostic evaluation of this patient?
- What is the most likely diagnosis and cause of this disease?

PAINE #PANCE Pearl – HEENT
Question
62yo man, with a history of pseudotumor cerebri, presents to your clinic with progressive headache and vision changes. You would like to confirm an increased intracranial pressure before sending him to the neurologist.
- What are two (2) ways at the bedside you can confirm and what are the thresholds for positive findings?
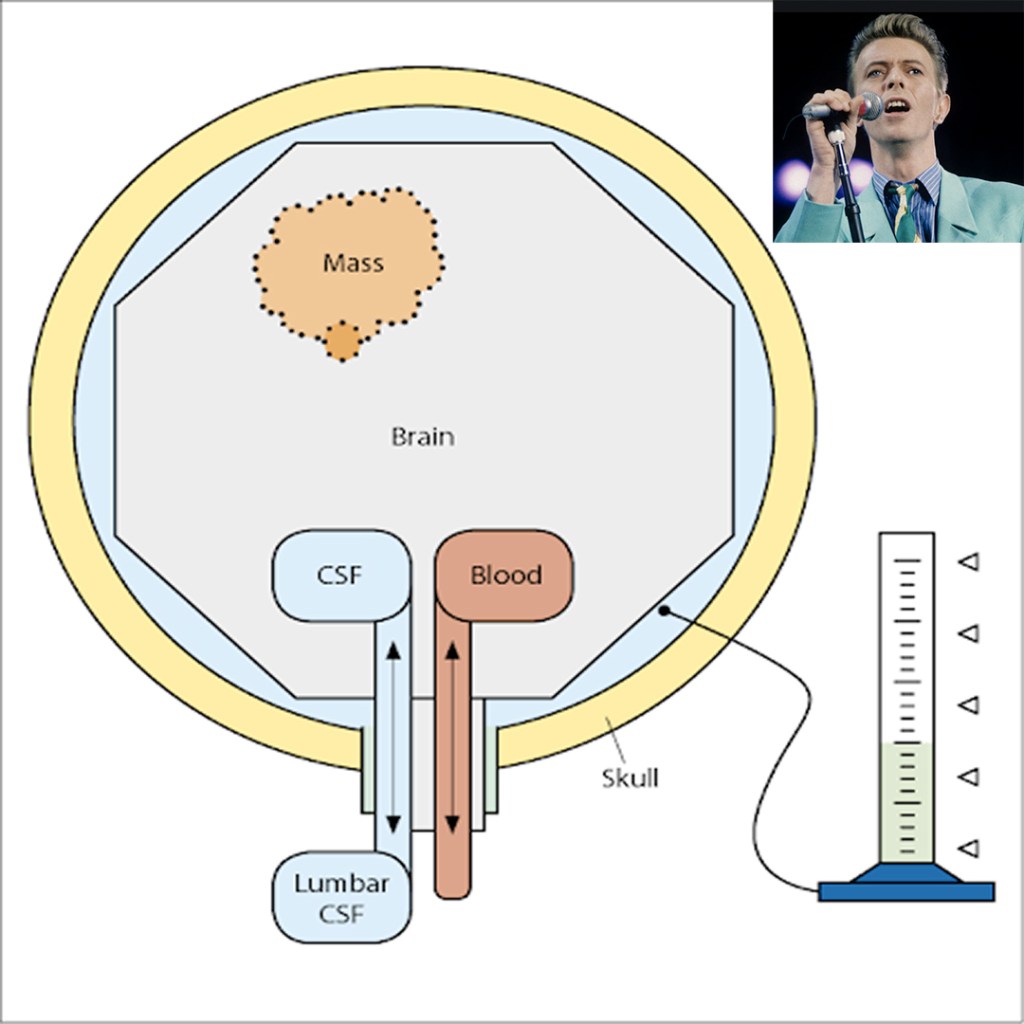
Answer
- The old and busted bedside way to determine if a patient has increased intracranial pressure is the fundoscopic examination. What you are looking for specifically is the cup:disc ratio of the optic nerve. Normal is around 0.3, or 1/3rd. If it is increased, it suggests increased intracranial pressure.
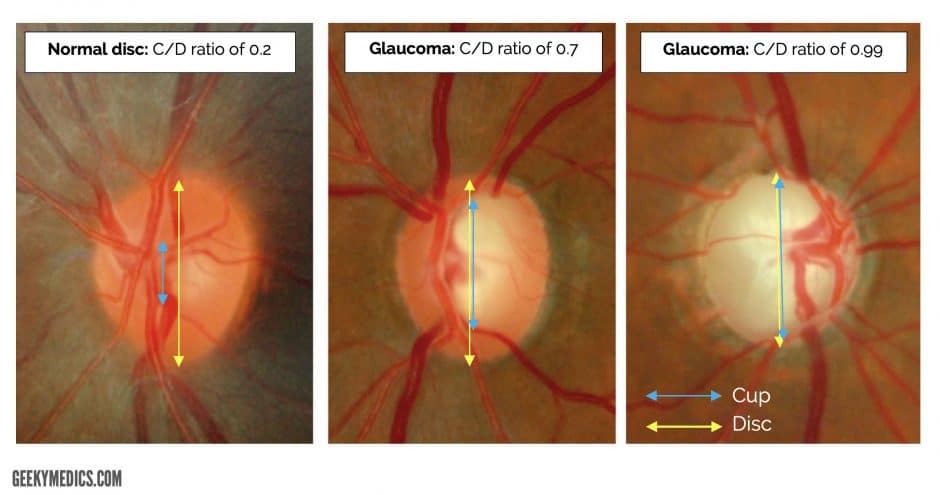
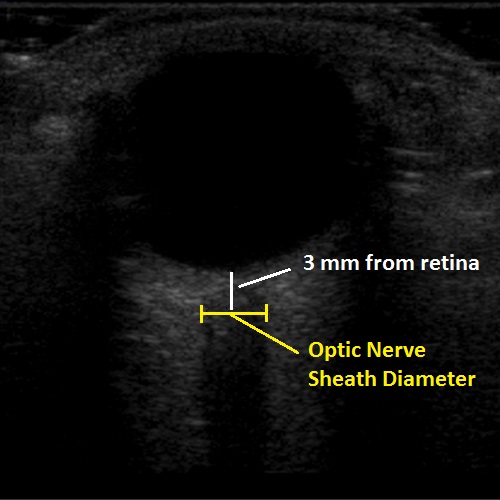
2. The new, hotness is using bedside POCUS to measure the optic nerve directly. Using the high frequency linear probe with a tegaderm placed over the patient eye, place a generous amount of gel over the globe and measure the optic nerve 3mm from the retina. A normal optic nerve should be < 5mm in diameter and anything over than suggests increased intracranial pressure
PAINE #PANCE Pearl – HEENT
Question
62yo man, with a history of pseudotumor cerebri, presents to your clinic with progressive headache and vision changes. You would like to confirm an increased intracranial pressure before sending him to the neurologist.
- What are two (2) ways at the bedside you can confirm and what are the thresholds for positive findings?