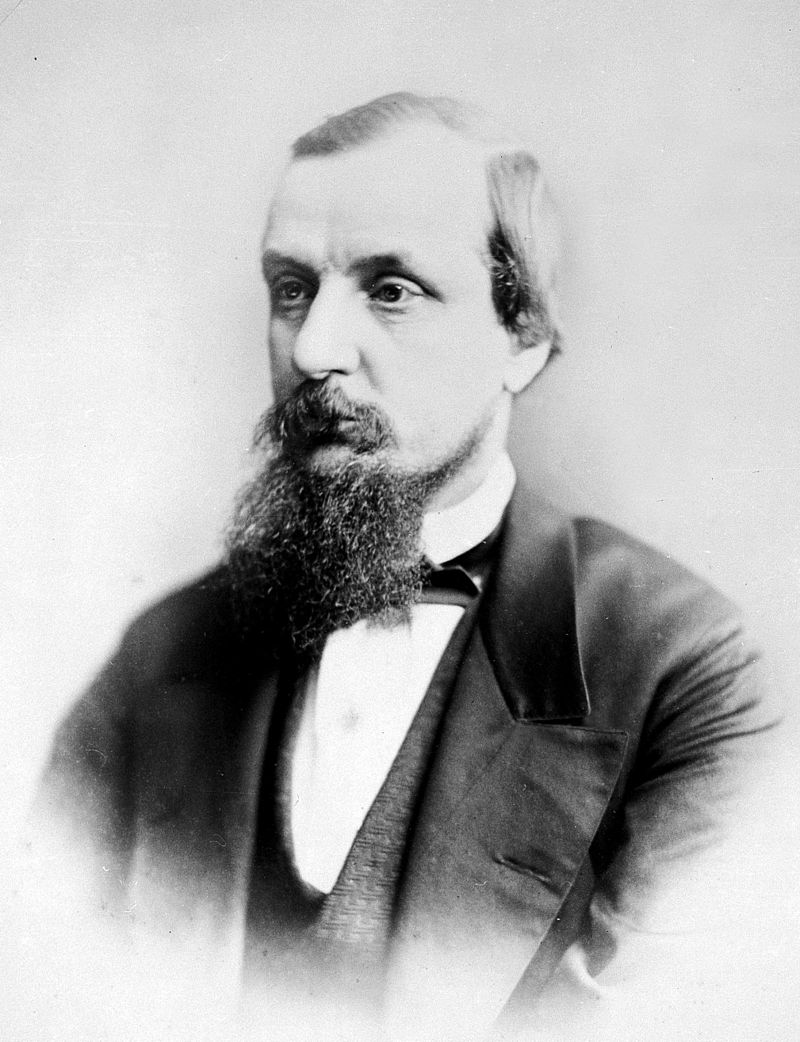Kocher Incision
Other Known Aliases – right subcostal incision
Definition – oblique incision in the right subcostal area starting 2-5cm below the xiphoid process, running parallel to the ribs, and extending to 2.5cm below the inferior costal margins
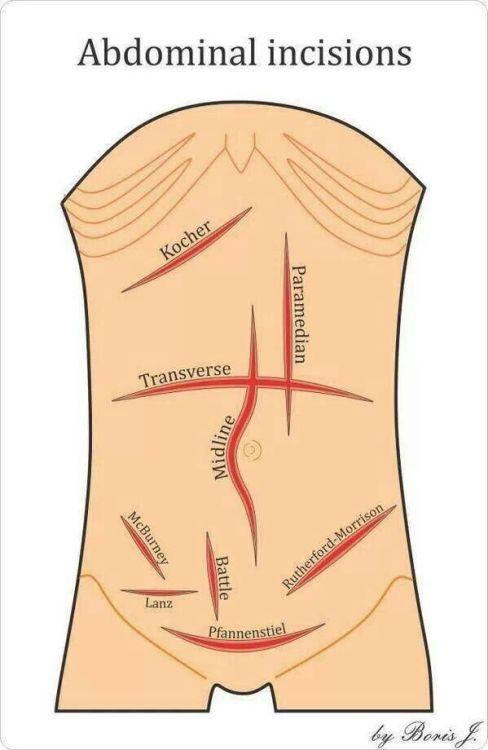
Clinical Significance – classic incision used for open cholecystectomy
Kocher Maneuver
Other Known Aliases – retroperitoneal exposure
Definition – maneuver to expose the retroperitoneal structure (pancreas, duodenum, vena cava)

Clinical Significance – this maneuver is used for resection of pancreatic head tumors or in trauma with retroperitoneal hemorrhage. The peritoneum is incised at the right edge of the duodenum and continued in a “C” shaped from superior to inferior. The duodenum and head of the pancreas is then reflected medially to the left to expose the retroperitoneal structures.

History – Named after Emil Theodor Kocher (1841-1917), a Swiss surgeon who obtained his medical doctorate from the University of Bern in 1865. He was arguably the most accomplished surgeon of his time and true pioneer in the field of surgery by promoting and advocating the use of aseptic technique, meticulous dissection with attention to minimal blood loss, and implementation of the scientific method in surgery. His “Text-Book of Operative Surgery” was the definitive guide to surgery in the early 1900s. He received the Nobel Prize in Physiology and Medicine in 1909…the first Swiss citizen and first surgeon to do so. The practice of modern surgery would certainly not be where it is today without the work of Dr. Kocher and his other notable eponyms are:
- Kocher forceps – hemostatic tooth and groove forceps
- Kocher’s point – entry point for intrventricular catheter to drain CSF from the cerebral ventricles
- Kocher-Debre-Semelaigne Syndrome – hypothyroidism in infancy
- Kocher collar incision – used in thyroid surgery
- Kocher’s sign – eyelid phenomenon in hyperthyroidism


References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
-
Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved
http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Kocher T. Text-Book of Operative Surgery. 1911. https://archive.org/details/textbookofoperat01kochuoft
-
Gautschi OP, Hildebrandt G. Emil Theodor Kocher (25/8/1841-27/7/1917)–A Swiss (neuro-)surgeon and Nobel Prize winner.
British journal of neurosurgery. 2009; 23(3):234-6. [
pubmed]
- Biography of Theodor Kocher by Nobel Prize Society. https://www.nobelprize.org/nobel_prizes/medicine/laureates/1909/kocher-bio.html

![]()
![]()