Surgery
PAINE PANCE Postcard – Hernias
Ep-PAINE-nym
Foramen of Winslow
Other Known Aliases – omental foramen, epiploic foramen
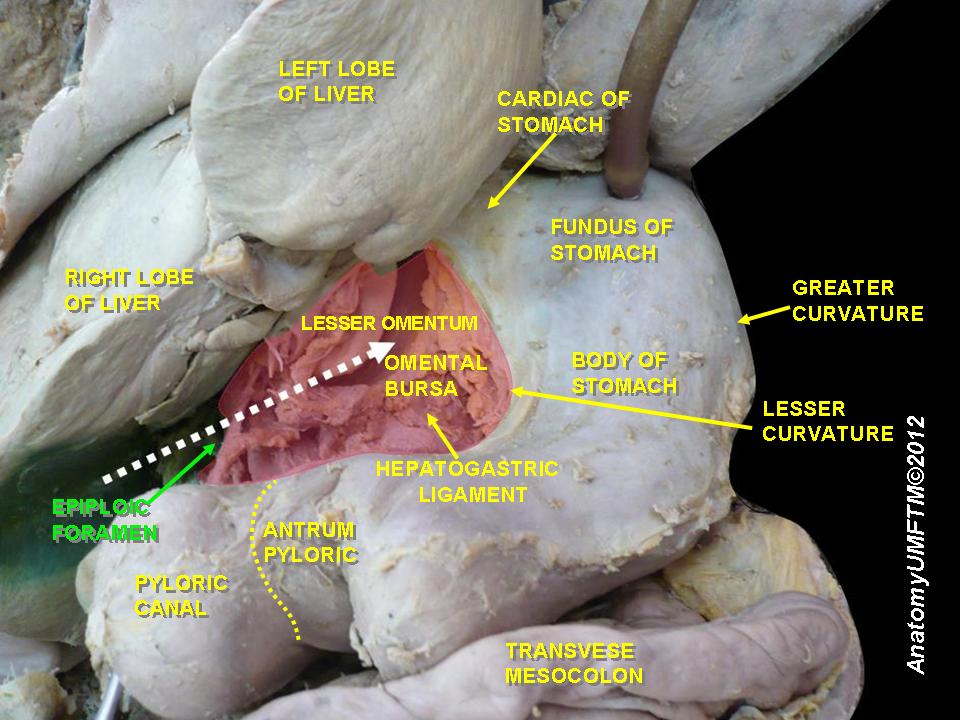
Definition – anatomic passage between the greater sac and the lesser sac of the abdomen

Clinical Significance – there are four anatomic borders of this communication:
- Anterior – hepatoduodenal ligament
- Posterior – peritoneum covering the IVC
- Superior – peritoneum covering the caudate lobe of the liver
- Inferior – peritoneum covering the commencement of the duodenum and hepatic artery
History – Named after Jacob Winslow (1669-1760), a Danish-born French anatomist who received his degree from Ole Borch’s College in 1693, while training under barber-surgeon Johannes de Buchwalde. He would concentrate on anatomy, instead of surgery, as the site of blood “alarmed him”. He would go on to train with many of the most revered surgeons and anatomists of his time while traveling Europe and was widely regarded as the greatest European anatomist of his day. His career would culminate in achieving professor anatomicus and full professor of anatomy at Jardin du Roi in 1743. His most famous work entitled “Exposition anatomique de la structure du corps humain” was published in 1732 and was the quintessential anatomical text of the mid-1700’s
References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- WInslow JB. Exposition Anatomique de La Structure Du Corps Humain. 1732 [link]
PAINE #PANCE Pearl – Surgery
Question
A 37yo man is presenting to your practice to establish primary care. He reports a history of controlled inflammatory bowel disease and sees a gastroenterologist every 6 months. Before you begin your physical examination:
- What are some of the identifiable extraintestinal manifestations of inflammatory bowel disease
Answer
A simple mnemonic for the extraintestinal manifestations of inflammatory bowel disease is A PIE SACK:
- Apthous ulcers
- Pyoderma gangrenosum
- Iritis
- Erythema nodosum
- Sclerosing cholangitis
- Arthritis or Ankylosing Spondylitis
- Clubbing of the fingers
- Kidney (amyloid deposits, nephrotic syndrome)

Ep-PAINE-nym
Pringle Maneuver
Other Known Aliases – none
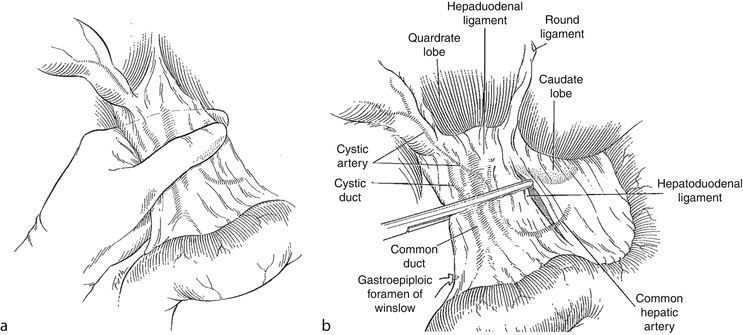
Definition – surgical technique whereby the hepatoduodenal ligament is clamped to limit blood flow through the hepatic artery and portal vein to the liver

Clinical Significance – the specific technique is to insert an index finger through the foramen of Winslow behind the porta hepatis and pinch between the finger and the thumb. You can also slide a non-crushing clamp along the finger, or wrap a vessel loop around to occlude. This technique controls the majority of the blood flow to the liver and is used to control bleeding during liver surgery or after liver trauma.
History – Named after James Hogarth Pringle (1863-1941), who was an Australian/Scottish surgeon and received his medical doctorate from the University of Edinburgh Medical School in 1885. He would have a prestigious career pioneering management and treatments for long bone fractures, head injuries, malignant melanomas, and reconstructive arterial surgery using vein grafts. He would describe his eponymous maneuver in 1908 in an article in the Annals of Surgery entitled “Notes on the Arrest of Hepatic Hemorrhage Due to Trauma”. It should also be noted that he was a fervent advocate for women in medicine, allowing them in his clinic well before any of his colleagues, and becoming Lecturer in Surgery and Demonstrator of Anatomy at Queen Margaret College, which was one of the first medical schools for women in Scotland.
References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Pringle JH. V. Notes on the Arrest of Hepatic Hemorrhage Due to Trauma. Ann Surg. 1908; 48(4):541-9. [PDF]
PAINE #PANCE Pearl – Surgery
Question
A 37yo man is presenting to your practice to establish primary care. He reports a history of controlled inflammatory bowel disease and sees a gastroenterologist every 6 months. Before you begin your physical examination:
- What are some of the identifiable extraintestinal manifestations of inflammatory bowel disease

Ep-PAINE-nym
Triangle of Calot
Other Known Aliases – none
Definition – anatomic space bordered by the cystic duct (inferiorly), common hepatic duct (medially) and cystic artery (superiorly)

Clinical Significance – this anatomic space is where you can see lymphadenopathy in patients with cholecystitis. This is often confused with the cystohepatic triangle (read more here).
History – Named after Jean-François Calot (1861-1944), who was a French surgeon and received his medical doctorate from Saine-Pe de Bigorre in 1880. He would go on to have a modest career in the field of orthopaedic surgery, and is known for describing the treatment of spinal deformities in Pott’s Disease. He would describe his eponymonic area in his doctoral thesis defense in 1891.

References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Calor JF, De la cholécystectomie. Doctoral thesis, Paris, 1891.
#69 – Benign Breast Diseases
***LISTEN TO THE PODCAST HERE***
Anatomy and Physiology
- Primary components of the breast are terminal duct lobular ubnits, lobular stroma, interlobular stroma, ducts, and lactiferous sinuses
- Epithelium (terminal duct lobular units) is the most hormonally responsive
- Natural hormonal changes of puberty, pregnancy, lactation, and menopause can lead to remodeling of these structures

Main Classifications
- There are four main classifications of benign breast disorders that are based on the degree of cellular proliferations and atypia present
- Nonproliferative
- Characterized by acinar dilation and fibrosis
- Generally, not associated with increased risk of cancer
- Proliferative without atypia
- Characterized by accumulation of luminal epithelial cells
- Small increased risk of cancer (1.5-2x general population)
- Atypical hyperplasia
- Change in size, shape, or nuclear function of epithelial cells
- High risk of cancer development
- Miscellaneous
- Nonproliferative
Epidemiology
- 50% of women will experience a non-cancerous breast mass at some point in their lives
- Age of diagnosis
- Mean age of 51 years
- Younger in proliferative
- Older in atypical
- Mean age of 51 years
- Family History
- Strongest in patients with atypical
NONPROLIFERATIVE DISORDERS
Breast Cysts
- Most common
- 25% of nonproliferative
- 35-50 year olds
- Fluid-filled, round mass originating from the terminal duct lobular unity
- Patient Presentation
- Painful or painless
- Often solitary
- Physical Examination
- Smooth and firm to palpation with distinct border
- Diagnostic Studies
- Ultrasound
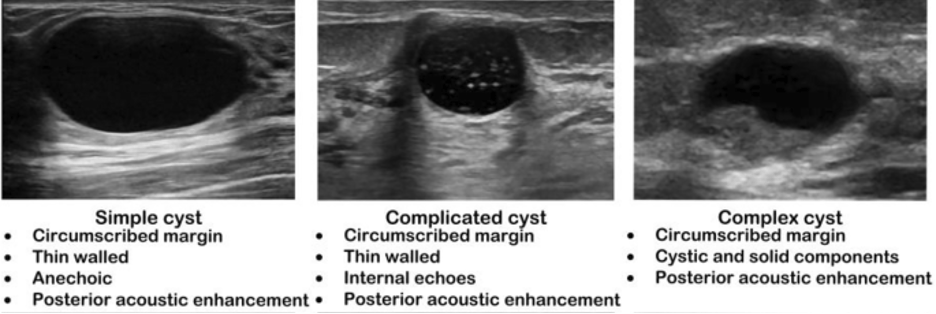
- Simple
- Anechoic throughout with posterior acoustic enhancement
- Complicated
- Homogenous low-level internal echoes with debris, thick walls, or thick septa
- No solid components
- Homogenous low-level internal echoes with debris, thick walls, or thick septa
- Complex
- Fluid and solid components without posterior wall enhancements
- Simple
- Ultrasound
- Management
- Simple – no intervention required
- Complicated – repeat imaging in 6 months
- Complex – biopsy or FNA
Galactocele
- Milk retention cysts usually caused by obstructed milk ducts
- Physical Examination
- Soft, cystic mass
- Diagnostic Studies
- Ultrasound
- Complex echogenicity
- Ultrasound

- Management
- FNA reveals milky substance
- No further intervention required
Hyperplasia of Usual Type
- Increase in the number of epithelial cells within a duct that is more than two, but not more than four cells in depth and do not cross the lumen of the involved space
PROLIFERATIVE DISORDERS WITHOUT ATYPIA
Fibroadenoma
- Most common benign tumor of the breast
- 50% of all breast biopsies
- 20% have multiple
- Most common in younger women
- 15-35 years of age
- Likely hormonally driven
- Persist through reproductive year’s, increase during pregnancy or with estrogen therapies, and decrease after menopause
- Physical Examination
- Well-defined, mobile mass on palpation
- Diagnostic Studies
- Ultrasound
- Well-defined solid mass with isoechogenicity
- Ultrasound

- Management
- Biopsy is indicated to further stratify
- Simple
- Contains glandular and fibrous tissue
- Watch vs excision vs cryoablation
- If any change during observation, then excision is warranted
- Complex
- Contains duct epithelial hyperplasia or calcification
- Observation vs excision
- Simple
- Biopsy is indicated to further stratify
Intraductal Papilloma
- Papillary cells that grown from the wall of a cyst into its lumen
- Can hide areas of atypia or ductal carcinoma in situ
- Two types
- Solitary
- Solid mass on examination or incidental imaging
- Nipple discharge is common presenting sign
- Multiple
- Minimum of five papillomas within a localized segment of tissue
- Solitary
- Diagnostic Studies
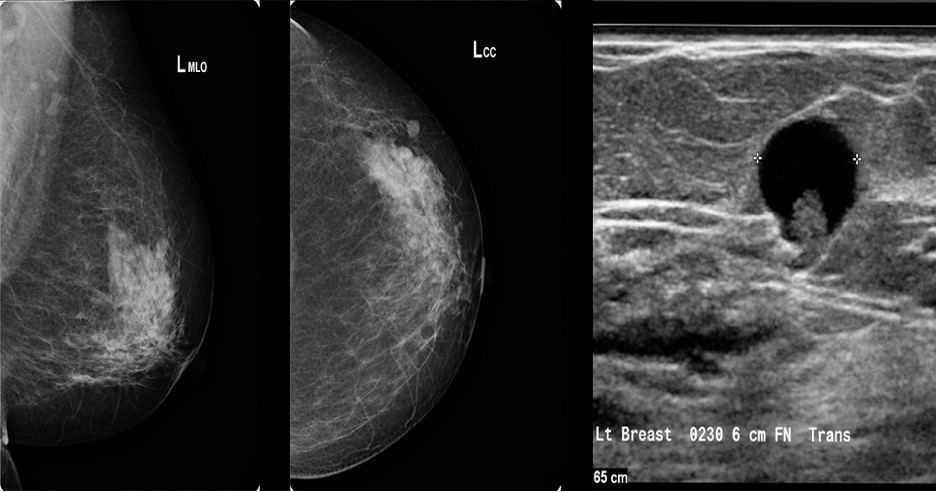
- Often found on routine mammography, but ultrasound is recommended if there is a palpable mass
- Will show a mass within a cystic space
- Often found on routine mammography, but ultrasound is recommended if there is a palpable mass
- Management
- Solitary
- Biopsy and excision if atypical cells present
- Multiple
- Excision of breast segment
- Solitary
Sclerosing Adenosis
- Lobular lesions with increased fibrous tissue and interspersed glandular cells
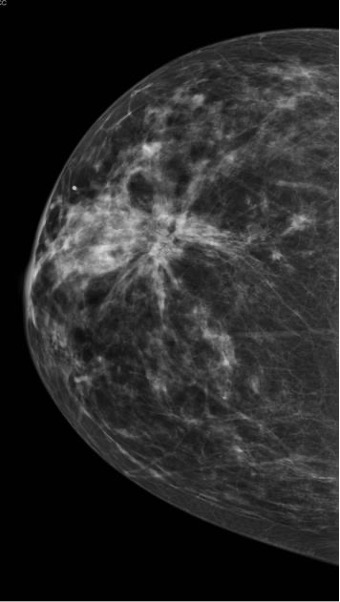
- Found on routine mammography
- Architectural distortion with irregular borders and microcalcifications
- No interventions needed outside of routine imaging
Radial Scar
- Complex sclerosing lesions found on routine imaging AFTER biopsies or excisions have been performed
- Pathologic by definition due to appearance
- Diagnostic Studies
- Mammography often shows low-intensity, spiculated masses that are indistinguishable from spiculated carcinomas
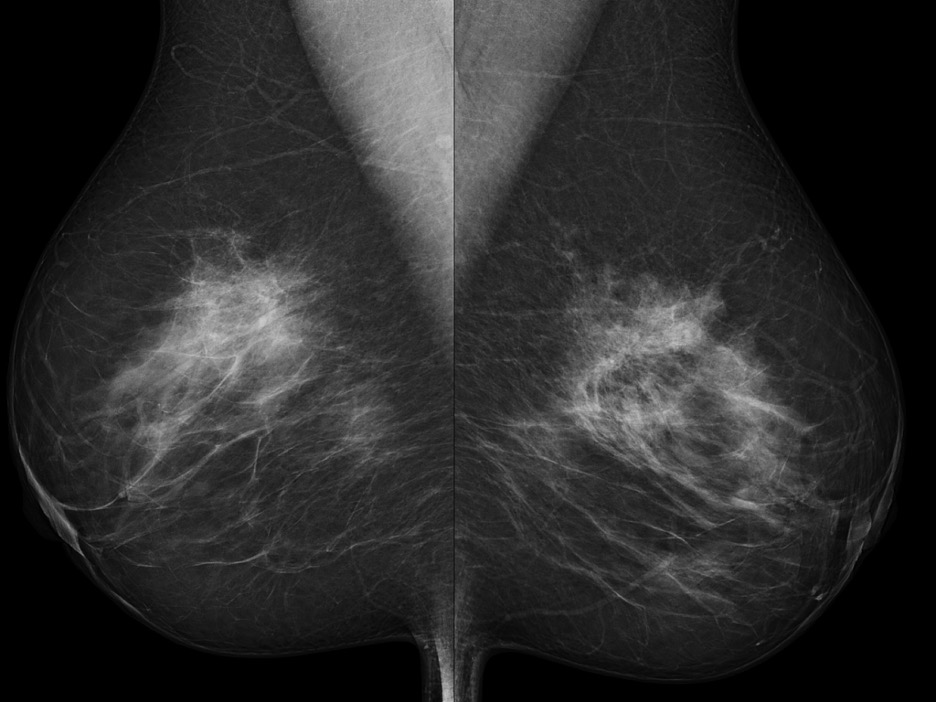
- Management
- Biopsy reveals fibroelastic cores with radiating ducts and lobules
- Excision is recommended (though controversial) and is often definitive
PROLIFERATIVE LESIONS WITH ATYPIA
Atypical Ductal Hyperplasia (ADH)
- Characterized by proliferation of uniform epithelial cells with monomorphic round nuclei filling the involved duct
- Must be < 2mm or involving < 2 ducts
- Can share cytologic and morphologic features of low-grade ductal carcinoma in-situ
- Diagnosed by core needle biopsy
- Management
- Excisional breast biopsy with good margins
Atypical Lobular Hyperplasia (ALH)
- Characterized by proliferation of monomorphic, evenly spaced, dyshesive cells filling the involved lobule
- Generally found on incidental biopsy for other clinical reason
- Can share cytologic and morphologic features of low-grade lobular carcinoma in-situ
- Diagnosed by core needle biopsy
- Management
- Excisional breast biopsy with good margins
Lobular Carcinoma in-situ
- Invasive lesion that arises from the lobules and terminal ducts of the breast
- 80-90% of cases diagnosed in premenopausal women with a mean age of 45 year’s
- Strong estrogen receptor positivity
- Diagnosed by core needle biopsy on other incidental reason
- LCIS is generally not diagnosed clinically, radiographically, or by gross pathologic examination
- Three types
- Classic
- Solid proliferation of small cells with small, uniform round nuclei and variably distinct cell borders with cytologic dyshesion
- Clear to lightly eosinophilic cytoplasm with possible signet ring cells and vacuoles
- Pleomorphic
- Larger cells with marked nuclear pleomorphism
- Florid
- Marked distension of the involved ducts and lobules that become mass-forming
- Central necrosis with calcifications
- Classic
- Management
- Excisional breast biopsy
Flat Epithelial Atypia
- Characterized by neoplastic alteration of the terminal duct lobular units with replacement of the native epithelial cells with columnar cells
- Diagnosed by core needle biopsy after mammographic evidence of microcalcifications
- Management
- Excisional breast biopsy
MISCELLANEOUS
Lipoma
- Solitary mature fat tumors of the breast that do not contain histologic evidence of breast tissue
- Physical Examination
- Soft, non-tender, well-circumscribed mass
- Difficulty to clinically differentiate from other conditions
- Soft, non-tender, well-circumscribed mass
- Excisional biopsy is preferred

Fat Necrosis
- Occurs as a result of breast trauma or surgical intervention
- Can be confused with malignancy both clinically and radiographically
- May see oil cysts on mammography or ultrasound
- Biopsy is often needed to diagnose, but no further treatment is indicated

Diabetic Mastopathy
- Seen in premenopausal women with long standing type 1 diabetes mellitus
- Mammogram shows dense pattern
- Diagnosed by core needle biopsy
- Shows dense, keloid-like fibrosis with periductal, lobular, or perivascular lymphocytic infiltration
- No further treatment after diagnosis
Hamartoma
- Lesions containing varying amounts of glandular, adipose, or fibrous tissue
- Present as discrete, encapsulated, painless masses found on incidental radiographic screening
- FNA or CNB are not sufficient to make the diagnosis and excisional biopsy is preferred
1893 Cottage Physician


References
- https://armandoh.org/disease/breast-cancer/
- Schnitt SJ. Benign breast disease and breast cancer risk: morphology and beyond. Am J Surg Pathol. 2003; 27(6):836-41. [pubmed]
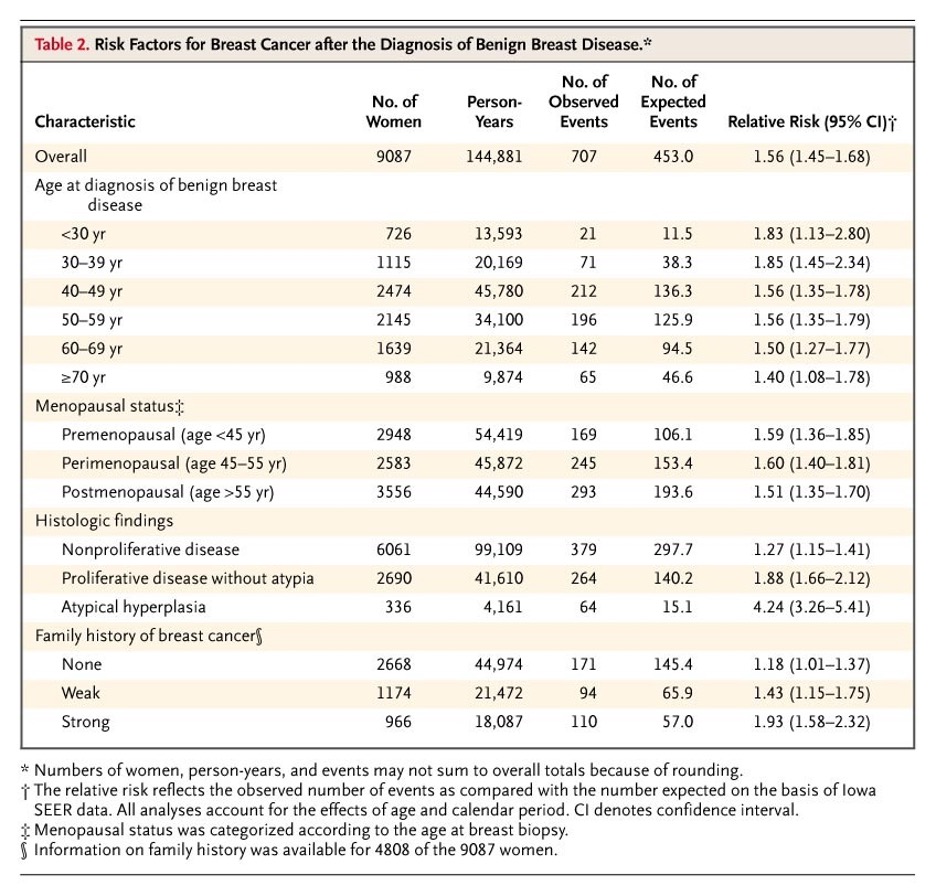
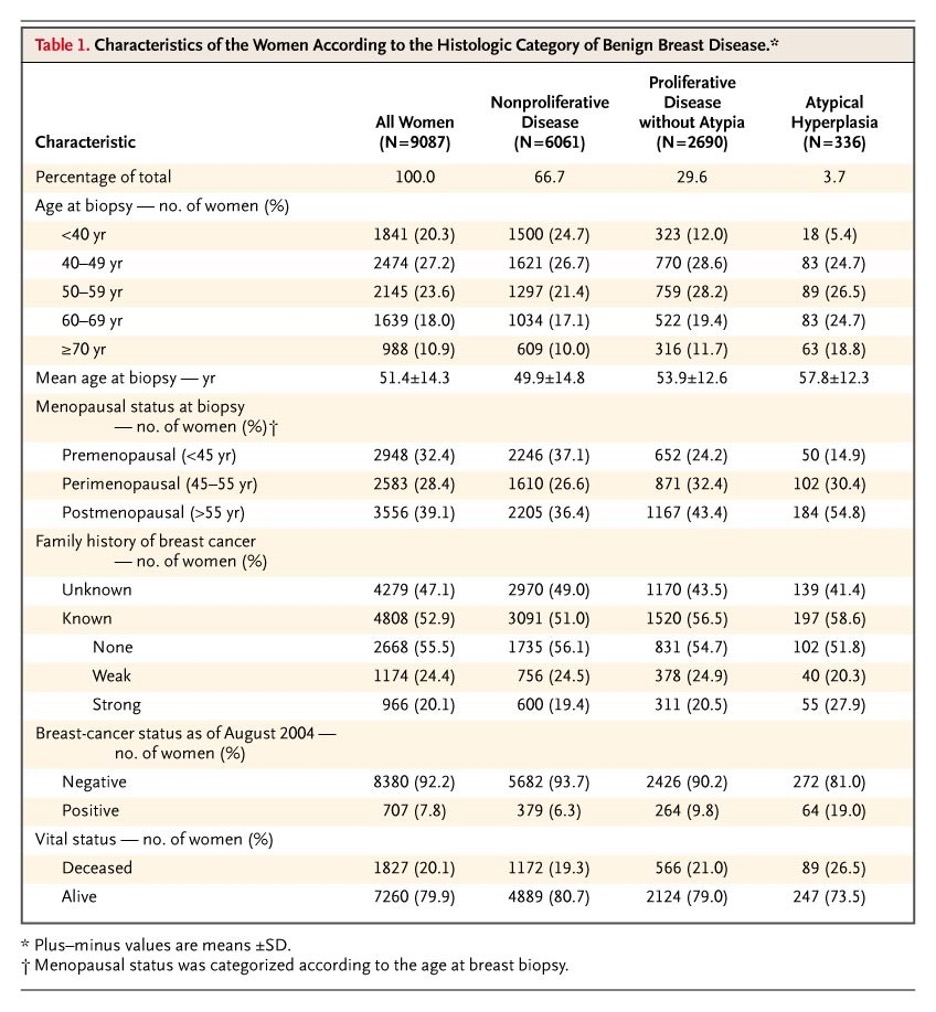
- Hartmann LC, Sellers TA, Frost MH, et al. Benign breast disease and the risk of breast cancer. N Engl J Med. 2005; 353(3):229-37. [pubmed]
- Guray M, Sahin AA. Benign breast diseases: classification, diagnosis, and management. Oncologist. 2006; 11(5):435-49. [pubmed]
- Breast Disease. In: Hoffman BL, Schorge JO, Halvorson LM, Hamid CA, Corton MM, Schaffer JI. eds. Williams Gynecology, 4e. McGraw-Hill; Accessed February 21, 2021. https://accessmedicine-mhmedical-com.ezproxy.uthsc.edu/content.aspx?bookid=2658§ionid=218608871
- Giuliano AE, Hurvitz SA. Breast Disorders. In: Doherty GM. eds. Current Diagnosis & Treatment: Surgery, 15e. McGraw-Hill; Accessed February 21, 2021. https://accessmedicine-mhmedical-com.ezproxy.uthsc.edu/content.aspx?bookid=2859§ionid=242155824
- Littrup PJ, Freeman-Gibb L, Andea A, et al. Cryotherapy for breast fibroadenomas. Radiology. 2005; 234(1):63-72. [pubmed]
- Linda A, Zuiani C, Furlan A, et al. Radial scars without atypia diagnosed at imaging-guided needle biopsy: how often is associated malignancy found at subsequent surgical excision, and do mammography and sonography predict which lesions are malignant? AJR Am J Roentgenol. 2010; 194(4):1146-51. [pubmed]
- American Society of Breast Surgeons. Official statement. Consensus guideline on concordance assessment of image-guided breast biopsies and management of borderline or high-risk lesions. 2016. Available at: https://www.breastsurgeons.org/docs/statements/Consensus-Guideline-on-Concordance-Assessment-of-Image-Guided-Breast-Biopsies.pdf
- Guray M, Sahin AA. Benign breast diseases: classification, diagnosis, and management. Oncologist. 2006; 11(5):435-49. [pubmed]
Ep-PAINE-nym
Puestow Procedure
Other Known Aliases – Puestow-Gillesby procedure, lateral pancreaticojejunostomy
Definition – side-to-side anastomosis of the main pancreatic duct of Wirsung to the proximal jejunum

Clinical Significance – this is a surgical management option for patients with chronic pancreatitis by simultaneously facilitating drainage and preserving physiologic function of the pancreas.
History – Named after Charles Bernard Puestow (1902-1973), an American surgeon who recieved his medical doctorate from the University of Pennsylvania in 1925. He would serve as a military surgeon during the 2nd World War and commanded the 27th Evacuation Hospital providing surgical services to wounded soldiers in Europe and North Africa. His commitment to the veteran population would continue after the war when he established the first surgical residency program based in a veterans hospitals in the United States in 1946. It was at Hines Veterans Hospital in Illinois where he and his partner, William Gillesby, would publish their experience and outcomes on 21 patients with chronic pancreatitis in 1958, which would lead to the creation of his eponymonic surgical procedure.
References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- Bosmia AN, Christein JD. Charles Bernard Puestow (1902-1973): American surgeon and commander of the 27th Evacuation Hospital during the Second World War. J Med Biogr. 2017; 25(3):147-152. [pubmed]
- PUESTOW CB, GILLESBY WJ. Retrograde surgical drainage of pancreas for chronic relapsing pancreatitis. AMA Arch Surg. 1958; 76(6):898-907. [pubmed]
PAINE #PANCE Pearl – Surgery
Question
Surgery is a major physiologic stress and often is accompanied by biochemical derangements that effect homeostasis in the post-operative period. Describe the most common clinical scenarios that can cause each of the four main acid-base imbalances in a post-surgical patient.
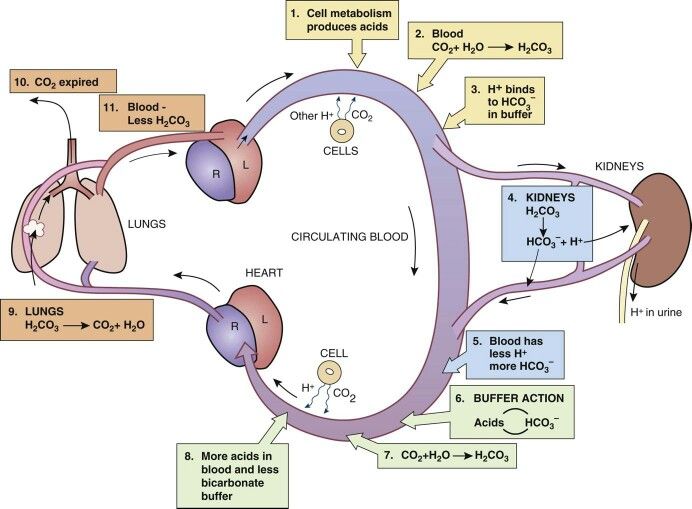
Answer
- Metabolic Acidosis
- Lactic acidosis (HAGMA)
- Under-resuscitation
- Blood loss
- Hyperchloremia (NAGMA)
- High chloride load from NaCl
- Lactic acidosis (HAGMA)
- Metabolic Alkalosis
- Volume contraction and bicarbonate reabsorption
- GI loss from NG tube suction or emesis
- Respiratory Acidosis
- Opioid medications causing depressed respiratory drive
- Respiratory Alkalosis
- Splinting from pain