Roux-en-Y Anastomosis
Other Known Aliases – end-to-end surgical anastomosis
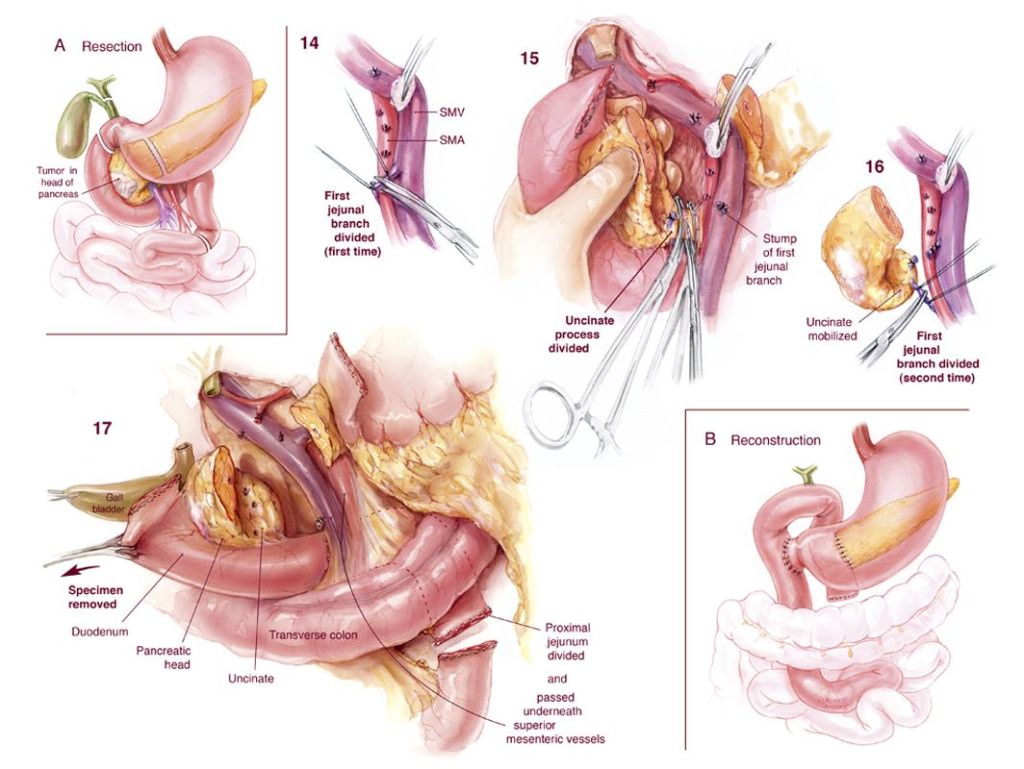
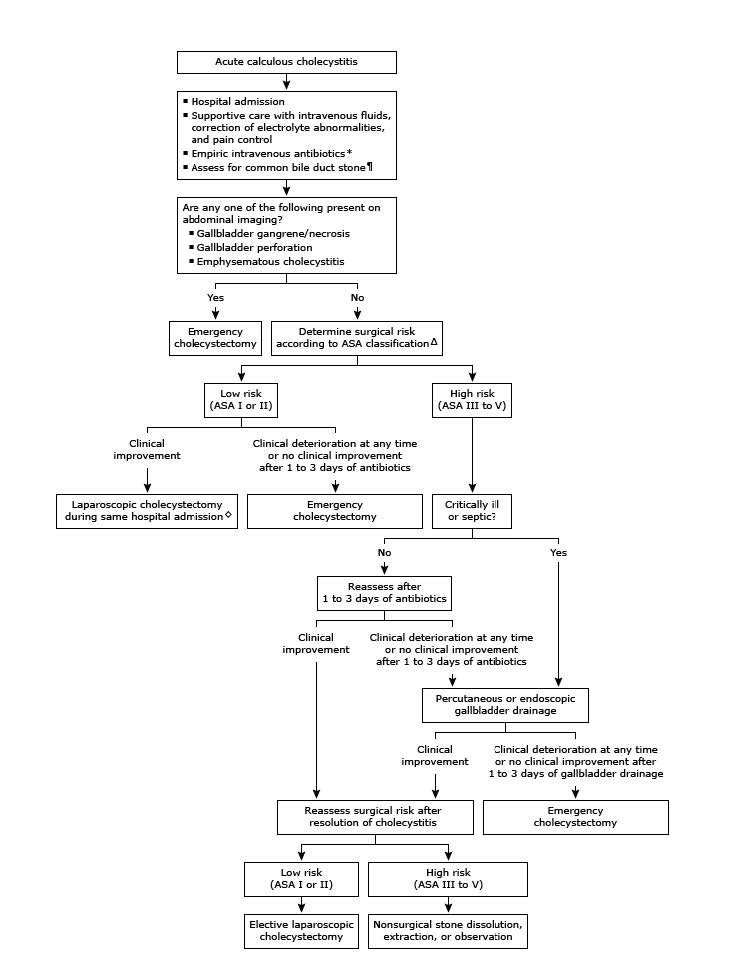
Definition – gastrointestinal tract is divided into two limbs (proximal, Roux limb and a distal limb) and are re-anastomosed farther down the GI tract, typically in the jejunum

Clinical Significance – this type of surgery is the traditional form of gastric bypass, where the proximal, Roux limb serves as the food reservoir and somach and the distal limb allows for physiologic drainage of gastric, hepatic, and pancreatic enzymes to aid in digestion. Other conditions it can be used is are chronic pancreatitis, alkaline gastritis, and various GI substitution procedures.

History – Named after César Roux (1857-1934), who was a Swiss surgeon and received his medical doctorate from the University of Bern 1880. He would stay on at his alma mater and assist Theodor Kocher until 1887, when he became chief of surgery at cantonal hospital of Lausanne. He would go on to have a modest career in surgery notable for two historical accomplishments. In 1893, he performed his eponymous procedure on a patient with gastric strictures from peptic ulcer disease to alleviate his obstruction symptoms. In 1926, the year of his retirement, he was the first surgeon to successfully remove a pheochromocytoma….7 months before Charles Mayo performed the same operation in the United States. Harvey Cushing visited his clinic in 1900 and said “he is a rough diamond-looks like Kipling-does excellent work and comes nearer to being the kind of man I am looking for than anyone else I have seen”.

References
- Firkin BG and Whitwirth JA. Dictionary of Medical Eponyms. 2nd ed. New York, NY; Parthenon Publishing Group. 1996.
- Bartolucci S, Forbis P. Stedman’s Medical Eponyms. 2nd ed. Baltimore, MD; LWW. 2005.
- Yee AJ, Pfiffner P. (2012). Medical Eponyms (Version 1.4.2) [Mobile Application Software]. Retrieved http://itunes.apple.com.
- Whonamedit – dictionary of medical eponyms. http://www.whonamedit.com
- Up To Date. www.uptodate.com
- C. Roux. De la gastroenterostomie. Revue de chirurgie, 1893, 13: 402-403.
- Hutchison R, Hutchinson AL. César Roux and His Original 1893 Paper. Obesity Surgery. 2010;20;953-956 [link]